The controversy surrounding penile rehabilitation after radical prostatectomy
Introduction
The American Cancer Society estimated that about 1 out of 7 men will be diagnosed with prostate cancer during his lifetime (1). However, 5-year survival rates after treatment of localized prostate cancer approximates 100%. The improvement and refinement in prostate cancer detection and treatment modalities have contributed to a younger patient population undergoing radical prostatectomy (RP) (2,3). Despite its efficacy in treating prostate cancer, RP has been shown to compromise erectile function (EF) and hence, the patient’s quality of life and general well-being (4).
Since the introduction of nerve-sparing techniques by Dr. Patrick Walsh in 1982, urologists can provide hope of regaining EF after RP. We currently have a better understanding of the distribution of the neurovascular bundles (NVBs) and cavernous nerves. Walsh initially stated that the NVBs had a symmetrical course through the posterolateral surface of the prostate (5). Later on, others discovered that NVBs may have either an anterolateral distribution or, occasionally, a posterolateral and lateral distribution on each side, respectively. These new concepts led to the technique of incision of the periprostatic fascia anteriorly and parallel to the NVBs to preserve both the posterolateral and anterolateral cavernous nerves covering the prostate (6-8).
Despite meticulous dissection in attempt to preserve the NVB during prostatectomy, there is evidence that neuropraxia, ischemic and hypoxic nerve insults, fibrotic remodeling, and apoptosis of cavernous smooth muscle contribute to ED (9,10). Neuropraxia is thought to arise from mechanical stretching of cavernous nerves, electrocautery-induced thermal injury and inflammation from surgical trauma. Chronic impotence reduces blood flow to the corporeal bodies, which leads to fibrosis and transformation of trabecular smooth muscle through collagen, which itself leads to the loss of the veno-occlusive mechanism required to maintain erections (10). Furthermore, ligation of accessory internal pudendal arteries during prostatectomy decreases arterial inflow which intensifies hypoxia and ultimately leads to apoptosis (10,11).
The introduction of the robot-assisted technology was considered to refine nerve-sparing procedures through three-dimensional magnification and movement calibration and many believed it would improve post-prostatectomy erectile dysfunction (ED) rates (12). Ficarra et al. (13) evaluated the prevalence and the potential risk factors of ED after robotic-assisted radical prostatectomy (RARP). The systematic review analyzed comparative studies which reported EF recovery outcomes on patients undergoing prostatectomy. For patients undergoing RARP, studies showed EF rates ranging from 54% to 90% and from 63% to 94% at 12- and 24-month, respectively. They performed a cumulative analysis of the studies evaluating the EF recovery 12 months after RARP or radical retropubic prostatectomy (RRP). This showed that when compared with RRP, RARP has a statistically significant advantage over RRP with an ED prevalence of 24.2% versus 47.8% in patients undergoing RRP at 12-month. They also suggested that age, baseline EF status, comorbidities, the use of athermal dissection and extension of the nerve-sparing procedure represent the most relevant or favorable preoperative and intraoperative predictors of EF recovery after RARP. However, Woo et al. (14) suggest that the current high rates of EF following RP are because of the introduction of phosphodiesterase type 5 inhibitors (PDE5Is) and not surgical technique.
Rehabilitation is one of the foundations in medicine today for the successful recovery in multiple diseases. Therefore, we believe penile rehabilitation should play a role in the postoperative management of patients who undergo RP. Penile rehabilitation consists of understanding the mechanisms that affect EF and utilizing pharmacologic agents, devices or interventions to promote male sexual function before and after any insult to the penile erectile physiologic axis (15,16). Despite the understanding of the mechanisms and well-established rationale for post-RP penile rehabilitation, there is still a big controversy regarding the effectiveness of rehabilitation programs. Our goal is to provide an update of the tools clinicians have available for penile rehabilitation after RP.
PDE5Is
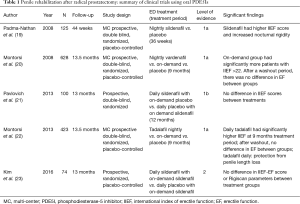
PDE5Is entered the market in 1998 and revolutionized the treatment of ED. PDE5Is have been shown to decrease the breakdown of cyclic guanosine monophosphate (cGMP) which then increases the efflux of intracellular calcium ions and result in smooth muscle relaxation and erection. This mechanism is potentiated by nitric oxide production stimulated by cavernous nerves (17,18). Clinical trials studying the use of PDE5Is after RP presented in this review are summarized in Table 1.
Full table
A number of studies have investigated the role of different PDE5Is in patients undergoing RP and many of these reported higher international index of erectile function (IIEF) scores and spontaneous erection rates (19,24-26). Padma-Nathan et al. (19) performed the first multicenter, double-blind, randomized, placebo-controlled trial to our knowledge investigating the effects of PDE5Is on EF after RP. They randomized 125 patients into three treatment groups: (I) placebo; (II) sildenafil citrate 50 mg; and (III) sildenafil citrate 100 mg. Out of the 125 patients, only 76 completed the post-8-week washout evaluation period. After the post-washout period, only one of 25 patients (4%) in the placebo arm had adequate EF, versus 14 of 51 patients (27%) in the sildenafil 50 and 100 mg groups combined (P=0.016). Although there was a significant dropout rate calling into question the statistical power of the study, they suggested that nightly sildenafil has a benefit for patients with post-prostatectomy ED.
Montorsi et al. (20) published the REINVENT trial in 2008. This multicenter, double-blind placebo-controlled trial randomized 628 patients with a baseline IIEF score of >26 into taking nightly vardenafil, on-demand vardenafil, or placebo for 9 months. After 9-month treatment period, on-demand vardenafil was associated with more patients obtaining ≥22 on the EF domain of the IIEF (IIEF-EF) score. Similarly, dropout rates were substantial, ranging between 31–35% in the study arms and there was no defined limit in the drug usage in the on-demand arm. Moreover, the data argued against the use of nightly PDE5I in the treatment of ED after RP.
Pavlovich et al. (21) pursued to investigate whether nightly sildenafil had an advantage over on-demand sildenafil. They randomized 100 men with good EF who had undergone nerve-sparing RP into two groups. The nightly sildenafil group consisted of patients taking nightly sildenafil and on-demand placebo; and the on-demand group consisted of on-demand sildenafil (with a maximum on-demand dose of 6 tablets per month) and nightly placebo starting the day after surgery for 12 months. All men had previously completed an IIEF-EF survey before surgery and had a score of ≥26 before undergoing nerve-sparing RP. Surgeons prospectively recorded the quality of NVB preservation, and this was quantified using a nerve sparing score (NSS) of one to four, with higher scores representing better preservation. The double-blind study period included quality of life assessments every 3 for 12 months after RP, and a final assessment at 13 months after a washout period of 1 month. Compliance in returning questionnaires ranged from 60–96% per time-point but was balanced between groups. After adjusting for potential confounding factors, no significant differences were found in EF between treatments at any single time-point after RP. NSS was the only factor that was consistently found to have a significant association with EF outcomes in all longitudinal multivariable models. This study did show some limitations. First, fearing that patients would not want to be randomized to a placebo-only group, a pure placebo arm was not part of the trial. Moreover, 90% of subjects were Caucasian which is not generalizable to all populations.
Unlike the previous trials, Mulhall et al. (27) found that 3 months of treatment with avanafil taken on-demand significantly improved drug-assisted EF after prostatectomy. They randomized 298 patients with post-prostatectomy ED of 6 months or more to on-demand 100 or 200 mg avanafil or placebo for 12 weeks. At the end of the treatment period, 31% of the 100 mg group and 41% of the 200 mg group responded that the treatment improved their erections when compared to placebo (10.7%). Dropout rates ranged from 8% to 24% between groups, with the largest amount in the placebo group in which 14 of 24 patients withdrew their consent. This fact raises the possibility that these patients perceived lack of treatment efficacy. However, follow-up was only for 3 months and long-term response to treatment or its effect on unassisted EF were not assessed in this trial.
A recent study by Montorsi et al. (22) aimed to compare the efficacy of tadalafil daily and on demand versus placebo in improving unassisted EF and reducing loss of penile length following nerve-sparing RP. Four hundred twenty-three were randomized into 9 months of treatment with tadalafil 5 mg once daily, tadalafil 20 mg on demand, or placebo followed by a 6-week washout period and 3 months open-label tadalafil once daily (to all patients). At 9 months, they found a significant difference in reaching target IIEF-EF ≥22 in the tadalafil once daily group compared to placebo. However, after the drug free washout period, there was no significant difference in EF between groups. After the open-label tadalafil once daily period, IIEF-EF scores increased in all treatment groups. Regarding penile length, there was significant protection from penile length loss in the daily tadalafil group (2.2 mm) compared to other groups (7.9 mm on demand, 6.3 mm placebo) at 9 months of treatment. These data suggest that PDE5Is may play a role in the preservation of cavernosal integrity by protecting against structural changes after nerve-sparing RP (22,28-31).
All these studies evaluated the use of PDE5Is by relying on self-reported outcomes to determine efficacy of therapy which could lead to response bias. Kim et al. (23) conducted a study to evaluate the effects of nightly sildenafil therapy using a more objective approach with nocturnal penile rigidity (RigiScan TM, Gotop Medical, Inc., St Paul, MN, USA) in addition to the IIEF-EF score. They randomized 97 patients of which 74 completed the study into taking daily sildenafil with on-demand sildenafil or daily placebo with on-demand sildenafil. Outcomes were evaluated every 3 for 12 months and at 13 months after 1 month wash-out period. They noted no significant difference in EF between treatment groups based on IIEF-EF domain or RigiScan, suggesting that nightly sildenafil has no benefit over on-demand sildenafil.
These trials open the debate on whether the use of PDE5Is makes a significant contribution to penile rehabilitation programs. All trials had a study period of 13 months or less, which is short of the 18–24 months duration recommended by some authors. Moreover, pharmacokinetics of each of the different PDE5Is has to be taken into consideration. Tadalafil has a longer half-life than other FDA approved PDE5Is used in these trials which could suggest a higher efficacy. In most of these studies, patients were operated either by open, laparoscopic or robot-assisted approach and results were given without separate statement of the outcomes for each technique (32). There still remains an opportunity for the development of larger trials with sufficiently long-term follow-up to convince the scientific community that PDE5Is play a role in penile rehabilitation.
Intracavernosal injection (ICI) and intraurethral therapy
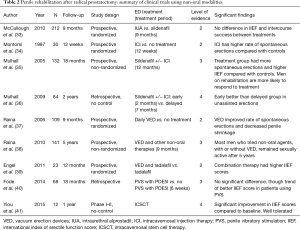
ICI and intraurethral therapy use alprostadil’s vasodilation effects to improve EF. Alprostadil delivers prostaglandin E1 (PGE1) which increases the levels of 3',5'-cyclic adenosine monophosphate (cAMP) within the erectile tissue and result in the efflux of intracellular calcium ions and cavernosal smooth muscle relaxation. Its intraurethral form generally does not cause systemic side-effects, but locally it can elicit urethral burning and penile pain (16,18,33). Trials investigating non-oral and non-pharmacological therapies are summarized in Table 2.
Full table
McCullough et al. (33) presented the first randomized, prospective trial to study the effect of intraurethral alprostadil (IUA) with Medicated Urethral System for Erection (MUSE, Vivus Inc., Mountain View, CA, USA). Two hundred and twelve men were randomized into taking nightly IUA or nightly sildenafil for 9 months. IUA was titrated from 125 to 250 µg after 1 month of treatment for better toleration of side effects. At study end, there was no statistically significant difference in the IIEF-EF score or successful intercourse rates. They did note a significant difference between groups in erections, assessed by the global assessment question, at 6 months in favor of IUA (76% vs. 60%). Although compliance rates were 98% and 79% for sildenafil and IUA, respectively, dropout rates approximated 30% for the IUA group secondary to pain experienced after the increase in IUA dosage.
The pioneers in penile rehabilitation strategies were Montorsi et al. (34) when they published the first clinical trial to evaluate ICI in 1997. They randomized 33 patients who underwent bilateral nerve-sparing RP to receive alprostadil injections 3 times per week for 12 weeks versus no treatment. After 6 months, 67% of men in the treatment group achieved spontaneous erections sufficient for penetration when compared to 20% in the control group.
Long-term trials evaluating ICI in penile rehabilitation are limited. Mulhall et al. (35) published a prospective non-randomized study on 58 men with good preoperative EF that were treated with early sildenafil, and if no EF response was noted, were transitioned to ICI 3 times per week. A control group consisting of 74 patients was allowed to have treatment on-demand but off-protocol. At 18 months after prostatectomy, 52% vs. 19% in the rehabilitation group and control group, respectively, reported unassisted spontaneous erections. In a similar study in 2009, Mulhall et al. (36) attempted to define if EF outcomes were better with early institution of therapy. They retrospectively evaluated 48 patients in the early group and 36 patients in the delayed group who were all instructed to obtain three erections per week using sildenafil initially, and if unsuccessful, use ICI. Penile rehabilitation started at mean time of 2 months in the early group and 7 months after RP in the delayed group. After 2 years, the group of patients who started rehabilitation earlier had a significant higher percentage of unassisted erections and IIEF-EF score >25. These studies unveil evidence that not only which therapy is offered, but the timing of penile rehabilitation is of paramount importance (16,36).
ICI and IUA have been found to contribute to EF recovery after RP. However, the literature still lacks well-designed randomized prospective trials with long-term follow-up to assess its overall effectiveness in penile rehabilitation.
Non-pharmacological therapies
The corpus cavernosum usually has low oxygen tension (PO2 =25–40 mmHg) during its flaccid state. When having an erection, the tension increases up to 90–100 mmHg which enables the release of NO and PGE1. These substances prevent collagen synthesis and fibrosis by suppressing transforming growth factor-beta 1 (TGF-β1) (42). The vacuum erection device (VED) causes an erection by creating negative pressure around the penis and drawing both venous and arterial blood into the corpus cavernosum. This increases both glanular and corporal oximetry, alleviates tissue hypoxia and prevents tissue fibrosis (43,44).
Raina et al. (37) were among the first to report VED use in patients undergoing RP. In their prospective clinical trial, they randomized 109 patients into using daily VED versus observation. In the VED group, 80% had erections sufficient for intercourse at 9 months and only 23% of those patients were less likely to report penile shrinkage.
Another prospective study by Raina and colleagues evaluated the effect of early use of VED in combination with sildenafil 100mg on-demand of 141 men after RP at 5 years. At 1- and 5-year follow-up, 80% and 62% of men were sexually active, respectively. After 5 years 71% of patients reported natural erections sufficient for intercourse, 8.5% were still using sildenafil, and 10% were using combination therapy of sildenafil plus VED (38). Unfortunately, this study had major limitations, as there was no control group and protocol details or nerve-sparing status were not revealed. Engel (39) did a similar study in which they randomized 23 patients undergoing bilateral nerve-sparing RARP into receiving tadalafil or tadalafil plus VED. Patients who had tadalafil plus VED had significantly higher IIEF-5 scores and greater penile hardness than the patients with PDE5I alone. After 1-year follow-up, 92% of the combination group reported engaging in vaginal intercourse versus 57% in the monotherapy group.
Penile vibratory stimulation is mostly used to stimulate an erection in men with ED and ejaculation in men with spinal cord injury. It works through the stimulation of branches of the pudendal nerves that lie along the penile shaft. The stimulation causes a reflex parasympathetic erection through the activation of nerve terminal endings that release nitric oxide and hence cGMP and cAMP that cause cavernosal smooth muscle dilation (45).
Fode et al. (40) reported the first human trial to investigate if PVS helps to recover EF in patients undergoing nerve-sparing RP. In their study, they randomized 68 patients into using PVS with oral PDE5Is versus oral PDE5Is alone. PVS consisted of stimulating the frenulum once daily for at least 1 week before surgery and for 6 weeks after catheter was removed. After 12 months, results showed that IIEF scores were higher in patients using the combination of PVS with oral PDE5Is, although no statistical difference was appreciated. Although they did not specify which type, frequency or dosage of the PDE5Is was used, this trial suggests that PVS may play a future role in penile rehabilitation.
Unlike PDE5Is, VED does not require intact corporal nerves and nitric oxide pathways for proper function. VED can warrant multiple erections on a daily basis early in the post-prostatectomy period, overcome RP-induced hypoxia, and prevent fibrosis that can lead to decrease in penile length and ED (16,46). The VED device contains a constriction ring used at the base of the penis that aids in maintaining erections for intercourse. However, blood gas analyses have shown hypoxia of penile blood after 30 minutes (47). Therefore, to prevent ischemic injury to the penis, a constriction ring should be avoided in penile rehabilitation unless the patient is planning vaginal intercourse. We believe that its low complication rates, lack of side effects and cost-effectiveness make VED a good addition to be taken into consideration while counseling patients for penile rehabilitation. The clinical trials investigating the use of VED and PVS showed that these non-invasive modalities are both acceptable and tolerable for patients.
Immunotherapy and stem cell therapy
Although the peripheral nervous system has the ability to regenerate after injury, this is usually limited and is not enough to prevent the pernicious effect on its end-organ function (48). Some researchers have analyzed strategies to improve regeneration and protection of cavernous nerves in order to reduce the time of denervation of the corpora cavernosa after injuries such as RP. These strategies have shown favorable results in animal models but have yet found their way into clinical practice (48,49).
In the early 2000s, several groups (50,51) discovered that immunomodulatory drugs can alleviate the inflammatory reaction that leads to cavernous nerve apoptosis and degeneration. These studies showed that immunophilin ligands can exert a neuroprotective effect on rats after cavernous nerve injury and maintain EF (52,53). However, the promising effects were not appreciated when these drugs were translated to clinical trials (54,55).
Bochinski et al. (56) was the first to report that neural embryonic stem cells preserved EF in rats that underwent cavernous nerve injury. Stem cells can undergo self-regeneration, differentiate into various phenotypes, and functionally and structurally regenerate injured or damaged tissues (57,58). Other researchers later validated these findings and after noticing that only a few labelled stem cells were found 4 weeks after injection, they concluded that adipose tissue-derived stem cells might exert their beneficial effects via a paracrine mechanism (59). Lin and colleagues recently attempted to counteract this ‘wash-out’ effect and found a way to keep injected stem cells in the corpus cavernosum by magnetizing these with NanoShuttle magnetic nanoparticles, hence improving EF even more after stem cell therapy (60).
Evidence from animal results suggests intracavernous injection of stem cells as a promising treatment approach for ED after RP. This has motivated researchers to initiate phase I and II clinical trials in humans. Yiou et al. (41) recently presented their phase 1–2 pilot clinical trial of intracavernous autologous bone marrow-mononuclear cell injection in patients undergoing RP. A total of 12 patients with localized prostate cancer and vasculogenic post-prostatectomy ED refractory to medical treatment were treated with escalating doses of stem cell therapy. As any phase I study, the primary endpoint was tolerance and secondary endpoints were the effects on EF assessed with IIEF scores and penile vascularization determined by Doppler ultrasound. After 6 months of the treatment, no adverse effects occurred. When compared to baseline, there was a significant improvement in IIEF scores. They also noted an increase in Doppler peak systolic velocity which was sustained after 1 year. Although no major beneficial conclusions could be drawn due to the lack of a control group, these studies suggest that stem cell therapy could play a role in penile rehabilitation in the future.
Conclusions
Several factors contribute to post-prostatectomy EF including age, pre-existing ED, medical comorbidities, surgeon techniques, equipment and experience. The purpose of penile rehabilitation is to preserve health and minimize damage to erectile tissue during the period of neural recovery by providing adequate oxygenation to the cavernous tissues (61). Ferrini et al. showed that PDE5I rehabilitation has a beneficial effect on penile tissue by preventing veno-occlusive dysfunction and on the major pelvic ganglia where the medication can ameliorate the production of damaging factors and increase the expression of favorable factors after cavernous nerve injury. These results proposed for the first time that PDE5Is may be used as a neuroprotective agent to alleviate neuropathic pain and favor neuroregeneration after RP (62,63).
Although there is not enough evidence to create an algorithm for penile rehabilitation, the use of most of the therapies and modalities reviewed in this article have been well-tolerated and no significant harm of rehabilitation has been demonstrated provided the patients understand the side-effects and costs of each modality. This has driven urologists in the United States to include penile rehabilitation programs in their practices (64). Most have adopted the therapies provided in our review, either monotherapy or a combination of different modalities. We noted that research in penile rehabilitation is leading towards the use of combination therapies. Some have started to evaluate the benefits of long-term PDE5Is in combination with stem cell therapy in rats undergoing cavernous nerve injury and found that there was complete recovery of EF in rats receiving dual therapy. When given PDE5Is or stem cell therapy alone, they observed only a partial erectile response (65). Others are even combining intracavernosal stem cell injections with newer modalities such as low-energy shockwave therapy to not only improve injured cavernous nerves, but also promote angiogenesis in the corpus cavernosum (66).
We believe penile rehabilitation should be a key component in the postoperative care of patients undergoing RP. Erectile recovery should not only be focused on penile function, but also aimed to establish a satisfactory and healthy sexual life for both the patient and their partners, regardless of whether there is complete restoration of spontaneous EF. Some researchers have suggested that the application of behavioral science methods and tools by a clinical sexologist, in addition to the standard medical/surgical EF care, can improve the ability to have regular sexual activity with penetrating sex in patients undergoing robotic RP (67,68). Although there is a controversy in the effectiveness of penile rehabilitation modalities, any rehabilitation is undeniably better than no action at all. By combining excellence in the technique of robotic-assisted RP with penile rehabilitation modalities, urologists can not only improve their patients’ chance of survival, but also their quality of life after surgery.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
References
- What are the key statistics about prostate cancer? American Cancer Society. Available online: http://www.cancer.org/cancer/prostatecancer/detailedguide/prostate-cancer-key-statistics. Last accessed on 2016 January 25.
- Bechis SK, Carroll PR, Cooperberg MR. Impact of age at diagnosis on prostate cancer treatment and survival. J Clin Oncol 2011;29:235-41. [Crossref] [PubMed]
- Welch HG, Albertsen PC. Prostate cancer diagnosis and treatment after the introduction of prostate-specific antigen screening: 1986-2005. J Natl Cancer Inst 2009;101:1325-29. [Crossref] [PubMed]
- Sanda MG, Dun RL, Michalski J, et al. Quality of life and satisfaction with outcome among prostate –cancer survivors. N Engl J Med 2008;358:1250-61. [Crossref] [PubMed]
- Walsh PC, Partin AW, Epstein JI. Cancer control and quality of life following anatomical radical retropubic prostatectomy: results at 10 years. J Urol 1994;152:1831-36. [PubMed]
- Menon M, Tewari A, Peabody J, et al. Vattikuti Institute prostatectomy: technique. J Urol 2003;169:2289-92. [Crossref] [PubMed]
- Kiyoshima K, Yokomizo A, Yoshida T, et al. Anatomical features of periprostatic tissue and its surroundings: a histological analysis of 79 radical retropubic prostatectomy specimens. Jpn J Clin Oncol 2004;34:463-8. [Crossref] [PubMed]
- Savera AT, Kaul S, Badani K, et al. Robotic radical prostatectomy with the “veil of Aphrodite” technique: histologic evidence of enhanced nerve sparing. Eur Urol 2006;49:1065-73; discussion 1073-4. [Crossref] [PubMed]
- McCullough AR. Rehabilitation of erectile function following radical prostatectomy. Asian J Androl 2008;10:61-74. [Crossref] [PubMed]
- Wang R. Penile Rehabilitation after radical prostatectomy: where do we stand and where are we going? J Sex Med 2007;4:1085-97. [Crossref] [PubMed]
- Mulhall JP, Slovick R, Hotaling J, et al. Erectile dysfunction after radical prostatectomy: Hemodynamic profiles and their correlation with the recovery of erectile function. J Urol 2002;167:1371-5. [Crossref] [PubMed]
- Ficarra V, Cavalleri S, Novara G, et al. Evidence from robot-assisted laparoscopic radical prostatectomy: a systematic review. Eur Urol 2007;51:45-55; discussion 56. [Crossref] [PubMed]
- Ficarra V, Novara G, Ahlering TE, et al. Systematic review and meta-analysis of studies reporting potency rates after robot-assisted radical prostatectomy. Eur Urol 2012;62:418-30. [Crossref] [PubMed]
- Woo SH, Kang DI, Ha YS, et al. Comprehensive analysis of sexual function outcome in prostate cancer patients after robot-assisted radical prostatectomy. J Endourol 2014;28:172-7. [Crossref] [PubMed]
- Hakky TS, Baumgarten AS, Parker J, et al. Penile rehabilitation: the evolutionary concept in the management of erectile dysfunction. Curr Urol Rep 2014;15:393. [Crossref] [PubMed]
- Clavell-Hernandez J, Wang R. Penile Rehabilitation following prostate cancer treatment: review of current literature. Asian J Androl 2015;17:916-22. [Crossref] [PubMed]
- Gontero P, Kirby R. Proerectile pharmacological prophylaxis following nerve-sparing radical prostatectomy. Prostate Cancer Prostatic Dis 2004;7:223-6. [Crossref] [PubMed]
- Alba F, Wang R. Current status of penile rehabilitation after radical prostatectomy. CML-Urology 2010;16:93-101.
- Padma-Nathan H, McCullough AR, Levine LA, et al. Randomized, double-blind, placebo-controlled study of postoperative nightly sildenafil citrate for the prevention of erectile dysfunction after bilateral nerve-sparing radical prostatectomy. Int J Impot Res 2008;20:479-86. [Crossref] [PubMed]
- Montorsi F, Brock G, Lee J, et al. Effect of nightly versus on-demand vardenafil on recovery of erectile function in men following bilateral nerve-sparing radical prostatectomy. Eur Urol 2008;54:924-31. [Crossref] [PubMed]
- Pavlovich CP, Levinson AW, Su LM, et al. Nightly vs on-demand sildenafil for penile rehabilitation after minimally invasive nerve-sparing radical prostatectomy: results of a randomized double-blind trial with placebo. BJU Int 2013;112:844-51. [Crossref] [PubMed]
- Montorsi F, Brock G, Stolzenburg JU, et al. Effects of tadalafil treatment on erectile function recovery following bilateral nerve-sparing radical prostatectomy: a randomized placebo-controlled study (REACTT). Eur Urol 2014;65:587-96. [Crossref] [PubMed]
- Kim DJ, Hawksworth DJ, Hurwitz LM, et al. A prospective, randomized, placebo-controlled trial of on-demand vs. nightly sildenafil citrate as assessed by Rigiscan and the international index of erectile function. Andrology 2016;4:27-32. [Crossref] [PubMed]
- McCullough AR, Levine LA, Padma-Nathan H. Return of nocturnal erections and erectile function after bilateral nerve-sparing radical prostatectomy in men treated nightly with sildenafil citrate: subanalysis of a longitudinal randomized double-blind placebo-controlled trial. J Sex Med 2008;5:476-84. [Crossref] [PubMed]
- Bannowsky A, Schulze C, Vander-Horst C, et al. Recovery of erectile function after nerve-sparing radical prostatectomy: improvement with nightly low-dose sildenafil. BJU Int 2008;101:1279-83. [Crossref] [PubMed]
- Pace G, Del Rosso A, Vicentini C. Penile rehabilitation therapy following radical prostatectomy. Disabil Rehabil 2010;32:1204-8. [Crossref] [PubMed]
- Mulhall JP, Burnett AL, Wang R, et al. A phase 3, placebo controlled study of the safety and efficacy of avanafil for the treatment of erectile dysfunction after nerve sparing radical prostatectomy. J Urol 2013;189:2229-36. [Crossref] [PubMed]
- Berookhim BM, Nelson CJ, Kunzel B, et al. Prospective analysis of penile length changes after radical prostatectomy. BJU Int 2014;113:E131-6. [Crossref] [PubMed]
- Nelson CJ, Scardino PT, Eastham JA, et al. Back to baseline: erectile function recovery after radical prostatectomy from the patients’ perspective. J Sex Med 2013;10:1636-43. [Crossref] [PubMed]
- Mostafa ME, Senbel AM, Mostafa T. Effect of chronic low-dose tadalafil on penile cavernous tisues in diabetic rats. Urology 2013;81:1253-9. [Crossref] [PubMed]
- Brock G, Motorsi F, Costa P, et al. Effect of Tadalafil once daily on penile length loss and morning erections in patients after bilateral nerve-sparing radical prostatectomy: Results from a randomized controlled trial. Urology 2015;85:1090-6. [Crossref] [PubMed]
- Schauer I, Keller E, Muller A, et al. Have rates of erectile dysfunction improved within the past 17 years after radical prostatectomy? A systematic analysis of the control arms of prospective randomized trials on penile rehabilitation. Andrology 2015;3:661-5. [Crossref] [PubMed]
- McCullough AR, Hellstrom WG, Wang R, et al. Recovery of erectile function after nerve sparing radical prostatectomy and penile rehabilitation with nightly intraurethral alprostadil versus sildenafil citrate. J Urol 2010;183:2451-56. [Crossref] [PubMed]
- Montorsi F, Guazzoni G, Strambi LF, et al. Recovery of spontaneous erectile function after nerve-sparing radical retropubic prostatectomy with and without early intracavernous injections of alprostadil: results of a prospective, randomized trial. J Urol 1997;158:1408-10. [Crossref] [PubMed]
- Mulhall J, Land S, Parker M, et al. The use of an erectogenic pharmacotherapy regimen following radical prostatectomy improves recovery of spontaneous erectile function. J Sex Med 2005;2:532-40. [Crossref] [PubMed]
- Mulhall JP, Parker M, Waters BW, et al. The timing of penile rehabilitation after bilateral nerve-sparing radical prostatectomy affects the recovery of erectile function. BJU Int 2010;105:37-41. [Crossref] [PubMed]
- Raina R, Agarwal A, Ausmundson S, et al. Early use of vacuum constriction device following radical prostatectomy facilitates early sexual activity and potentially earlier return of erectile function. Int J Impot Res 2006;18:77-81. [Crossref] [PubMed]
- Raina R, Pahlajani G, Agarwal A, et al. Long-term potency after early use of a vacuum erection device following radical prostatectomy. BJU Int 2010;106:1719-22. [Crossref] [PubMed]
- Engel JD. Effect on sexual function of a vacuum erection device post-prostatectomy. Can J Urol 2011;18:5721-5. [PubMed]
- Fode M, Borre M, Ohl D, et al. Penile vibratory stimulation in the recovery of urinary continence and erectile function after nerve-sparing radical prostatectomy: a randomized, controlled trial. BJU Int 2014;114:111-7. [Crossref] [PubMed]
- Yiou R, Hamidou L, Birebent B, et al. Safety of intracavernous bone marrow-mononuclear cells for postradical prostatectomy erectile dysfunction: an open-dose escalation pilot study. Eur Urol 2016;69:988-91. [Crossref] [PubMed]
- Kim N, Vardi Y, Padma-Nathan H, et al. Oxygen tension regulates the nitric oxide pathway. Physiological role in penile erection. J Clin Invest 1993;91:437. [Crossref] [PubMed]
- Lin HC, Yang WL, Zhang JL, et al. Penile rehabilitation with a vacuum erectile device in an animal model is related to an antihypoxic mechanism: blood gas evidence. Asian J Androl 2013;15:387-90. [Crossref] [PubMed]
- Welliver RC Jr, Mechlin C, Goodwin B, et al. A pilot study to determine penile oxygen saturation before and after vacuum therapy in patients with erectile dysfunction after radical prostatectomy. J Sex Med 2014;11:1071-7. [Crossref] [PubMed]
- Stein MJ, Lin H, Wang R. New advances in erectile technology. Ther Adv Urol 2014;6:15-24. [Crossref] [PubMed]
- Qian SQ, Gao L, Wei Q, et al. Vacuum therapy in penile rehabilitation after radical prostatectomy: review of hemodynamic and antihypoxic evidence. Asian J Androl 2016;18:446-51. [Crossref] [PubMed]
- Bosshardt RJ, Farwerk R, Sikora R, et al. Objective measurement of the effectiveness, therapeutic success and dynamic mechanisms of the vacuum device. Br J Urol 1995;75:786-91. [Crossref] [PubMed]
- Weyne E, Castiglione F, Van der Aa F, et al. Landmarks in erectile function recovery after radical prostatectomy. Nat Rev Urol 2015;12:289-97. [Crossref] [PubMed]
- Bella AJ, Lin G, Cagiannos I, et al. Emerging neuromodulatory molecules for the treatment of neurogenic erectile dysfunction caused by cavernous nerve injury. Asian J Androl 2008;10:54-9. [Crossref] [PubMed]
- Sezen SF, Hoke A, Burnett AL, et al. Immunophilin ligand FK506 is neuroprotective for penile innervation. Nat Med 2001;7:1073-4. [Crossref] [PubMed]
- Lagoda G, Sezen SF, Burnett AL. FK506 and Rapamycin neuroprotect erection and involve different immunophilins in a rat model of vavernous nerve injury. J Sex Med 2009;6:1914-23. [Crossref] [PubMed]
- Hayashi N, Minor TX, Carrion R, et al. The effect of FK1706 on erectile function following bilateral cavernous nerve crush injury in a rat model. J Urol 2006;176:824-9. [Crossref] [PubMed]
- Valentine H, Chen Y, Guo H, et al. Neuroimmunophilin ligands protect cavernous nerves after crush injury in the rat: new experimental paradigms. Eur Urol 2007;51:1724-31. [Crossref] [PubMed]
- A safety and efficacy study of prograf in the prevention of erectile dysfunction after radical prostatectomy. Available online: http://clinicaltrials.gov/show/NCT00106392. Last accessed on 2016 Jan 29.
- Evaluate the effects of GPI1485 on erectile function following bilateral nerve-sparing prostatectomy. Available online: http://clinicaltrials.gov/show/NCT00090376. Last accessed on 2016 Jan 29.
- Bochinski D, Lin GT, Nunes L, et al. The effect of neural embryonic stem cell therapy in a rat model of cavernousal nerve injury. BJU Int 2004;94:904-9. [Crossref] [PubMed]
- Zhang H, Albersen M, Jin X, et al. Stem cells: novel players in the treatment of erectile dysfunction. Asian J Androl 2012;14:145-55. [Crossref] [PubMed]
- Shan H, Chen F, Zhang T, et al. Stem cell therapy for erectile dysfunction of cavernous nerve injury rats: a systematic review and meta-analysis. Plos One 2015;10:e0121428. [Crossref] [PubMed]
- Albersen M, Fandel TM, Lin G, et al. Injections of adipose tissue-derived stem cells and stem cell lysate improve recovery of erectile function in a rat model of cavernous nerve injury. J Sex Med 2010;7:3331-40. [Crossref] [PubMed]
- Lin H, Dhanani N, Tseng H, et al. Nanoparticle improved stem cell therapy for erectile dysfunction in a rat model of cavernous nerve injury. J Urol 2016;195:788-95. [Crossref] [PubMed]
- Mulhall JP, Morgentaler A. Controversies in sexual medicine: penile rehabilitation should become the norm for radical prostatectomy patients. J Sex Med 2007;4:538-43. [Crossref] [PubMed]
- Hlaing SM, Garcia LA, Kovanecz I, et al. Sildenafil promotes neuroprotection of the pelvic ganglia neurons after bilateral cavernosal nerve resection in the rat. BJU Int 2013;111:159-70. [Crossref] [PubMed]
- Garcia LA, Hlaing SM, Gutierrez RA, et al. Sildenafil attenuates inflammation and oxidative stress in pelvic ganglia neurons after bilateral cavernosal nerve damage. Int J Mol Sci 2014;15:17204-20. [Crossref] [PubMed]
- Tal R, Teloken P, Mulhall JP. Erectile function rehabilitation after radical prostatectomy: practice patterns among AUA members. J Sex Med 2011;8:2370-6. [Crossref] [PubMed]
- Martínez-Salamanca JI, Zurita M, Costa C, et al. Dual strategy with oral phosphodiesterase type 5 inhibition and intracavernosal implantation of mesenchymal stem cells is superior to individual approaches in the recovery of erectile and cavernosal functions after cavernous nerve injury in rats. J Sex Med 2016;13:1-11. [Crossref] [PubMed]
- Jeon SH, Shrestha K, Kim RY, et al. Combination therapy using human adipose-derived stem cells on the cavernous nerve and low-energy shockwaves on the corpus cavernosum in a rat model of post-prostatectomy erectile dysfunction. Urology 2016;88:226.e1-9. [Crossref] [PubMed]
- Ljunggren C, Ströberg P. Improvement in sexual function after robot-assisted radical prostatectomy: A rehabilitation program with involvement of a sexual sexologist. Cent European J Urol 2015;68:214-20. [Crossref] [PubMed]
- Skrodzka M. Sexual rehabilitation or penile rehabilitation – do we have an optimal post-prostatectomy regimen? Cent European J Urol 2015;68:221-2. [Crossref] [PubMed]


