Female genital mutilation/cutting in Africa
Introduction
Female genital mutilation (FGM), also known as female circumcision (FC), but more recently as female genital mutilation/cutting (FGM/C) according to the World Health Organization (WHO), has occurred in many forms in all societies (1).
It involves imposed incisions or excisions on and of the female external genitalia for sociocultural as opposed to medical reasons. Some authors have described it as a form of gender-based torture (2). The social scientist, Ellen Gruenbaum observes in The Female Circumcision Controversy, the difficulties in naming correctly the procedures performed, advising of the extreme caution required in answering the question why FGM/C is practised (3). FGM/C cuts across ethnicities and religious backgrounds, even though religious scholars claim that the holy books do not prescribe the practice. It has been outlawed in the Western world, but their immigrant populations have significant proportions of circumcised females from Africa, parts of Middle East, Asia and the Pacific (4,5). In a 2016 report, Teixeira and Lisboa estimated that in Portugal there may be over 6,500 immigrant women 15 years or older who have been circumcised and 1,830 girls under 15 years who are likely to or have undergone circumcision (4). Similarly, the study by Koukkula et al. in Finland demonstrated the burden of FGM/C among immigrant populations in developed nations with 69% and 32% of women of Somali and Kurdish origins respectively, who had been circumcised (6). Reports have shown that up to 140 million girls and women had undergone FC around the world in 2000; however it is now estimated to be about 200 million in 2016 (7,8).
FGM/C has been associated with wide ranging medical, economic, sociocultural and women rights consequences and is presently receiving global, multifaceted attention to eradicate the practice albeit with slow progress over the years (9,10).
Origin of FGM
The exact origin of FGM/C is not well-known but documented reports, Greek historians and geographers, such as Herodotus (425–484 B.C.) and Strabo (64 B.C.–23 A.D.) point out that FC occurred in Ancient Egypt along the Nile Valley at the time of the Pharaohs and thus Egypt is often considered as the source country (11). The act of FGM/C was also reported long time ago among other nations of the world including the Romans where it was done in order to prevent their female slaves from getting pregnant (12).
In Western Europe and the United States, clitoridectomy was described to be practiced so as to treat perceived ailments like hysteria, epilepsy, mental disorders, masturbation, nymphomania and melancholia in the 1950’s (13).
Types
Depending on cultures, traditions, customs and religion, there is a wide range of procedures performed and it is not known what percentage of which is practiced where. In some areas what is now done is just a ceremony simulating FGM/C and not actual surgical procedures (3).
According to WHO, FGM/C is defined as “all procedures involving partial or total removal of the external female genitalia or other injury to the female genital organs for non-medical reasons.” In the medical literature, four main types of FGM/C are recognized:
- Type I: excision of the clitoral hood with or without removal of parts or the entire clitoris (clitoridectomy);
- Type II: excision of the clitoris together with parts or all of the labia minora;
- Type III: excision of parts or the whole of the clitoris, labia minora and labia majora and stitching or narrowing of the introitus, with a very small outlet for passage of urine and menstruum. This is also known as infibulation;
- Type IV: other harmful procedures to the female genitalia for non-medical purposes. Examples are—pricking, piercing, incising, scraping and cauterization. Others are hymenectomy, cutting of the vagina and introduction of corrosive substances or herbs into the vagina to cause bleeding or to tighten or narrow the vagina.
Prevalence in Africa
The practice of FGM/C in Africa is one that has persisted due to strong sociocultural influences which ensure that it is secretly done and underreported particularly since the last two centuries. Curiously, it is one practice that is embraced by practitioners of all the major faiths prevalent on the continent—Christianity, Islam and traditional worship. Thus its extent is usually estimated and documented figures have been considered to be far less than what they are.
FGM/C is performed at varying age groups, from the first week of life, during infancy, before puberty, before the first childbirth and other periods in the woman’s life dependent on the location and major reason underlying the practice (8,14). It is usually performed individually but can be done in groups of girls or women. In Africa, the country specific rates are shown in Table 1, from studies done by the United Nations’ Children Fund (8). The body further projects that over the next decade 30 million girls less than 15 years old are at risk of FGM/C.
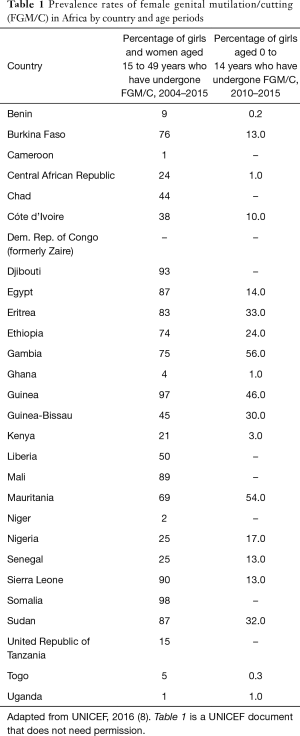
Full table
Within each country, there are wide differences in the types of procedure and prevalence of practice as the state—specific figures by Ngianga—Kandala et al. in 2009 (15) reveal for the states in Nigeria, in Table 2. These figures contrast with those obtained in 2013 for the same geopolitical zones of the country but by the fourth Nigeria Demographic and Health Survey (16) (Table 2). It is essentially for this reason that community specific interventions are mandatory in order to eradicate FGM/C.
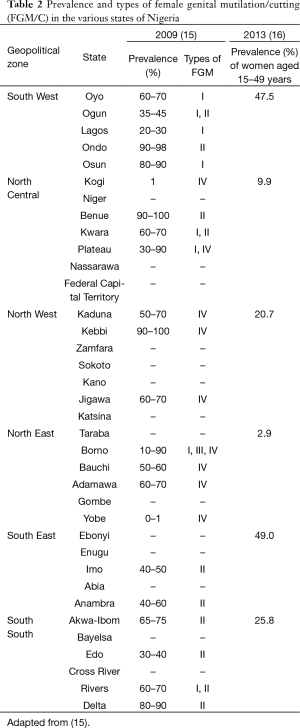

Full table
Reasons for performing FGM/C
Even though a major reason for FC is control of female sexuality, researchers in Kenya and Nigeria observed no association between FC and outcomes for sexual behaviour and concluded that sexual chastity is insufficient to justify the practice (17). Numerous other reasons have been adduced for the sustenance of the practice spanning tradition, religion and politics. Viewing FGM/C from an economic angle, for the practitioners, it serves as an income earner and for some families it is used to improve the marriage prospects of young girls. In some societies, it is used as a kind of social stratification mechanism with those who have been circumcised perceived to be at a higher status than others and is a prerequisite for the right to inheritance (9,13). Still others perform the procedures for anatomic/aesthetic judgements, prevention of child mortality or for hygiene reasons (9). However, evidence has not supported any medical benefits.
Instruments and methods used for FGM/C
The instruments used in performing FGM/C have included razor blades, unsterilized sharpened kitchen knives, scissors, glass, sharpened rocks and finger nails (18). The person who performs the procedure is often called the circumciser or cutter. In most cases, this is an older woman who does it in the house of the girl or woman, or in circumcision centres. In some communities, it is performed by males, usually barbers because of their skills in handling cutting tools.
Unhygienic procedures are commoner among the traditional circumcisers with the report of repeated use of a single instrument in up to 30 girls (19). In some countries of Africa and Asia such as Egypt, Kenya, Sudan and Indonesia, health professionals often perform the procedures and so it is termed “medicalization” of FGM/C (20-22). Anaesthesia is not used by traditional cutters but medical professionals may use local or general anaesthetic agents (23,24). When the procedure is performed by traditional cutters and especially in types II and III, the girl or woman’s legs are usually bound together from the hip to the ankle so she remains immobile for approximately 40 days to allow for the formation of scar tissue (25).
Payments for services
Most circumcisers or cutters collect modest remunerations which could be monetary or in form of gifts though some see it as a public service to their community (26,27). In Sudan and Egypt, it is customary to compensate the circumcisers with gifts and share the food and meat sacrificed during the circumcision feasts with them (26). In other settings where health care providers perform FGM/C, they do it either due to the erroneous belief that the procedure is safer when medicalized or because of the economic benefits (8,26). This is one of the reasons why its eradication has met with a lot of obstacles since it is a source of income with rather high fees in countries where it is illegal (26,27).
Cost of FGM/C
The costs of FGM/C include not only the price paid for the services but also the cost of treatment of its medical and related obstetric complications (28,29). As much as 1% of government expenditure is spent on the health of women in the reproductive age group as a result of FGM/C-related obstetric complications annually (29). In addition, a loss of 130,000 life years which is equivalent to losing half a month from each lifespan is expected due to complications of FGM/C related to obstetric haemorrhage with a total of $3.7 million spent in six African countries in a year (29). This is not limited to the monetary value since the psychosocial and emotional effects and their consequences on the family might be unquantifiable.
Complications
On account of the poor surgical skills of most practitioners of FGM/C, the absence of antiseptic techniques and non-use of anaesthetic agents, the procedures are associated with several complications. These sequelae may occur during or immediately after the operations, while others manifest in the medium and long-term to cause poor quality of life for the patient or result in mortality or both. The immediate complications include excruciating pain (when anaesthetic agents are not used), haemorrhage, shock, acute urinary retention, injury to adjacent tissues and death (9,27). A meta-analysis utilizing 185 studies in 57 countries where FGM/C is done detailed the most common immediate complications as excessive bleeding, urine retention and genital tissue swelling (30). For those who survive, medium term complications are infections of the reproductive tract following use of unsterilized or poorly sterilized instruments, septic techniques and septic environment and raw wound surfaces. All these result in urinary tract infection, pelvic inflammatory disease, chronic pelvic pain, infertility and ectopic pregnancy. Others are tetanus infection, infections with hepatitis and human immunodeficiency viruses and also abscess formation (9,27).
Among those who survive the acute and medium term consequences, many long-term morbidities noted are psychological disturbances, low libido, apareunia or dyspareunia, chronic pain, dysmenorrhoea, gynaetresia, cryptomenorrhoea, vaginal fistulae, labial agglutination, hypertrophic scar/keloids, clitoridal retention cysts, dermoid cysts, vaginal lacerations during coitus, straining at micturition, genital tract lacerations, especially during vaginal delivery, obstructed labour, increased rate of caesarean delivery and postpartum haemorrhage (31,32). Mortality can still occur following the above complications of labour and the puerperium. For the babies conceived by such women, there is increased risk of stillbirth, early neonatal death or babies with neurologic deficits from severe birth asphyxia (32).
The clitoris has extensive innervations and it plays crucial roles in sexual arousal, attainment of orgasm and sexual satisfaction. Its amputation or wholesome removal during FGM/C has been demonstrated to affect these functions. A validated questionnaire, the Female Sexual Function Index (FSFI) has been used by workers in France to determine the sexual, physical and psychological effects of FGM/C (33). Though the number studied was small, the instrument promises to help in the scientific evaluation of these patients.
Management of complications
Given the extent of these complications, the best management is to prevent the occurrence of FGM/C. When it has occurred, the line of management includes responding to the patient-specific complications. This is best done with a multidisciplinary approach and dependent on the time relation of the complications in the individual patient. When patients present in acute emergencies, rapid and skillful resuscitation techniques are imperative to keep them alive in addition to limiting medium and long-term complications. When haemorrhage occurs, ensuring haemostasis along with quick restoration of cardiovascular volume with crystalloids, blood and blood products and administering supplemental oxygen is crucial. For infections, a wound swab should be taken for microscopy, culture and sensitivity and the patient treated initially with potent broad spectrum antibiotics which may be changed if the sensitivity pattern so indicates. When laboratory facilities are unavailable, there should not be delay in commencing antibiotic therapy. Urethral catheterization with adequate analgesics will be helpful in the control of pain and acute urinary retention.
Following type III FGM/C, defibulation can be performed. This is a midline incision of the vulval scar, made on its anterior part. It may be performed during gynaecological procedures like cervical biopsy, during delivery or before delivery with the quest to prevent acute intrapartum problems such as obstructed labour or varying types of genital fistulae. Psychotherapy is extremely helpful for these women; good emotional support will help them overcome much of the challenges they have. Gynaetresia may require vaginoplasty, depending on severity. Keloids or hypertrophic scar not big enough to disturb sexual function may be left untouched; however large ones especially those causing difficulty during sexual intercourse, or with the possibility of causing obstructed labour will need to be managed by a plastic surgeon (32). Lower genital tract cysts can be managed by excision or marsupialization. Menstrual disorders such as dysmenorrhoea should be evaluated for severity and possible cause. Incision and drainage may be needed to relieve vulval abscesses (31). Fistulae and urinary incontinence are managed by urogynaecologists.
At the community level, other measures include improving health services in rural areas where the practice is more rampant, development of emergency care, referrals to a sex therapist and management of labour by well-trained medical and nursing personnel. Development of guidelines on management and creating help lines is also helpful, especially when accessing these lines is toll-free.
The midwife and the gynaecologist/obstetrician are poised more than other practitioners to manage circumcised women. Therefore these health care workers need additional training to enable case identification, reduce the obstetric and psycho-social effects of FGM/C, and prevent reinfibulation and the occurrence of new cases (34). Also of importance in the care of these patients are urological nurses, psychologist-psychotherapists, sexologists and social workers (5,35). The training of these health care practitioners needs to be well structured for them to cope (35).
In order to care effectively for girls/women who have had FGM/C, it is necessary to have accurate estimation of those affected or likely to undergo the procedures. The Royal College of Nursing has advocated improved information sharing on FGM/C across health and social care services in order to achieve this (36).
In school age girls who have been circumcised or face the risk of circumcision, the school nurse is in a vantage position to deliver educational and support services in developed countries while dedicated female teachers can perform these roles in resource challenged places (37).
Clitoral reconstructive surgery has been done with good effects. Vital et al. in France demonstrated a statistically significant improvement in median FSFI summary score of 29 from a preoperative score of 17 (P=0.009), although 75% of their patients had only type 2 mutilations (33). Similarly, Abramowicz et al. showed that 88% to 96% of their study participants expressed satisfaction with anatomic and psychosexual improvement following reconstruction (38).
In the case of adult patients of FGM/C or those likely to undergo the procedures, detailed information and counselling (DIC) has been shown to work. Abdulcadir et al. in Geneva, Switzerland examined eight East African women who requested for postpartum infibulation, but after DIC which lasted over 1 year, none except one persisted with the request (39). The factors that may have contributed to success were being away from a conducive environment for reinfibulation and the health resources of the country of emigration.
Effect of FGM/C on sexual satisfaction
One of the cultural and religious reasons for justifying the practice of FGM/C is in the reduction of promiscuity and ensuring virginity before marriage. While attempting to achieve its presumed benefit through reduction in sexual drive and desire it has a negative impact on the overall woman’s sexual life. FGM/C deprives women of sexual satisfaction and denies them of their right to sexual health and pleasure to achieve full psychophysical well-being (40). Circumcised women have reported several sexual problems including reduction in sexual desire, arousal, excitement, orgasm and dyspareunia at varying levels (41,42).
The level of sexual dissatisfaction among circumcised women depends on the types of circumcision. Women with types II, III and IV are more likely to experience increased sexual dissatisfaction because of lower levels of sexual functioning, decreased arousal, vaginal dryness during intercourse, and orgasm with increased pain and decreased overall satisfaction than those with type I FGM/C (43,44). In type III, also known as infibulation, the husbands’ inability to penetrate into the vagina can result into anal intercourse or even using the urethral meatus as an opening (25,45). However, some studies showed that most circumcised women with type I agreed FGM/C reduces orgasm markedly but does not totally eliminate sexual pleasure (40,43).
An association has been found between the female genital self-image and sexual function and behaviour with women that undergo types II, III and IV genital circumcision having negative genital image and much more likely to experience sexual dysfunction (46,47). This is corroborated by Krause et al. who documented improved sexual desire, arousal, and satisfaction following defibulation surgeries through the use of FSFI (48). A systematic review on FGM and sexual problems revealed women who have undergone FGM are 1.5 times more likely to experience dyspareunia and are twice likely to report a lack of sexual desire (49).
Effect of FGM/C on psychosocial health
The psychological effects of FGM/C depend on the type of the procedure performed, experience of the circumciser and the social atmosphere at the time the cutting is performed (45,50). The psychosocial consequences include post-traumatic stress disorder (PTSD), anxiety disorders, panic disorders, inhibition, depression and suppression of feeling and thinking and sometimes attempted suicide (40,45,51). These effects are due to psychological trauma of the painful procedure, sense of humiliation and being betrayed by parents, use of physical force by those performing the procedure, negative genital image, lack of sense of ownership of their bodies, devastating sexual life, infertility and vesicovaginal fistulae (40,45,51-53).
Women with type III FGM/C have a more distressing psychosocial complication in relation to sexual problems and infertility with a documented infertility rate of 30% (42,44). The purported infibulated scar that ought to protect from pregnancy out of wedlock and enhance men’s sexual pleasure serve as the impediment to conception within marriage and sexual pleasure thus causing an unhealthy sexual relationship and creates the fear that the women may never become mothers while their husbands question their masculinity (54). These account for 16.3% of divorce and marital discord in a study among circumcised women (55).
On the contrary, FGM/C provides a psychological relief to a child who is made to believe and celebrate the cultural act in the community where female genitals are seen as dirty or a source of enthralling temptation. The female child feels satisfied despite the pain, of being made clean and marriageable like every other female in the community rather than becoming despised and made the target of ridicule with no one in the community to marry her (56).
Effect of FGM on reproductive health
FGM/C has adverse effects on the reproductive health of circumcised women. It may cause partial or complete occlusion of the vaginal opening resulting in dysmenorrhea, haematocolpos, haematometria (45). Infertility results from FGM/C due to the consequences of pelvic infections or coital problems and when the circumcised women get pregnant they have higher risks of obstetric complications (32,45).
Circumcised women have increased risks of adverse events during labour and delivery with negative effects on their newborn babies (31,32). These risks increase with the severity of type of FGM and include postpartum hemorrhage, episiotomies, perineal lacerations, prolonged second stage of labour, operative vaginal delivery, caesarean deliveries, prolonged maternal hospital stay, infant resuscitation, stillbirth, or neonatal death (32,57,58). Infibulation may cause obstructed labour and is associated with an increased risk of vaginal/vulval lacerations and sometimes women with infibulation have defibulation performed at the time of delivery (59). In the Gambia, women with FGM/C are 4 times more likely to have complications during delivery, and their newborns are 4 times more likely to have health complications (60).
In the WHO’s study on delivery outcomes among 28,393 women with singleton pregnancies admitted for delivery at 28 obstetric centres in six African countries, a higher neonatal death rate was found among circumcised compared to non-circumcised mothers (32). Neonatal death rate was 15% higher for those whose mothers had type I, 32% higher for those with type II and 55% higher for those with type III FGM/C with an estimate of additional one to two babies per 100 deliveries dying as a result of FGM/C (32). Women who do not deliver in hospitals will have more severe obstetric complications with increased neonatal adverse outcome.
Effect of FGM and fistula
FGM/C could be directly or indirectly linked to fistula. Fistula could occur during FGM procedures or defibulation. It can cause prolonged obstructed labour which predispose to obstetric fistulae (45,51). Browning reported that types I and II FGM/C are not independent causative factors in the development of obstetric fistulas from obstructed labour but could not ascertain the relationship of type III FGM/C with obstructed labour. The author documented women with type III FGM/C presenting with fistula after delivery by traditional birth attendants who might have extensively cut the infibulated genitalia and the urinary tract at the time of delivery (61).
Prevention
The morbidities and mortalities associated with FGM/C are enormous without any medical benefits to the patients particularly in the resource poor countries where the practice occurs mostly. Therefore, its prevention and eradication are mandatory for human rights and socioeconomic reasons. Fortunately, the prevention of FGM/C is receiving the deserved global, local and grassroots attention. However, efforts need to be focused on using strategies to build evidence and generate knowledge, to increase advocacy, enforce legislation against FGM/C and strengthen the health sector’s response (7,51).
The first step should involve location specific researches to gather baseline community information, detail human and material resources that are available for the control of FGM/C and determine the best methods of prevention in that community. It is now universally agreed that methods of prevention must be holistic consisting of advocacy, general education especially of women, health education and promotion services, trade substitution ventures for the practitioners and legislation usually as the last resort. Also, emphasis should be placed on religious leaders advocating against the practice since it is associated with religious beliefs and they are well respected and have a great influence on their constituents (62).
In countries where the procedures are performed, the attitude of significant stakeholders such as husbands and fathers is important in eradicating the practice. Studies show that men who are against FGM/C can identify its physical, obstetric, psychological, sexuality and social consequences while those who support the practice generally deny the existence of these problems (63). Ten point three percent of women interviewed in Kenya supported the continuation of the practice (64).
Egypt used to have high rates of FGM. It has now recorded great declines in prevalence rates largely through mothers’ education and empowerment but also as a result of socioeconomic development of its communities (65). The Egypt Demographic and Health Surveys documented that 90% of girls up to 13 years used to be circumcised but this has now reduced to 28% in 2005 amongst girls aged 0–17 years and 18% in 2014 (66).
Recently in Egypt (Modrek and Liu) and in Kenya (Achia) it was demonstrated that women empowerment, particularly education, significantly affects the likelihood of the daughter becoming circumcised (64,67). But other factors related to the socioeconomic status and anti-FGM/C messages in the social media account for the decline in the practice of FGM/C (67).
Nongovernmental organizations have been in the forefront and have contributed immensely to the successes achieved so far in the care of girls/women who have been circumcised and in preventing the procedures from being carried out. These have included the United Nations’ International Children’s Emergency Fund (UNICEF) which in 1980 announced that its anti-FGM program is “based on the belief that the best way to handle the problem is to trigger awareness through education of the public, members of the medical profession and practitioners of traditional health care with the help of local collectives and their leaders”. Others are WHO, Inter-African Committee on Traditional Practices Affecting the Health of Women and Children, the 1994 United Nations’ International Conference on Population and Development (ICPD) in Cairo, Egypt and so on.
The government has a great responsibility in preventing FGM/C, in promoting its abandonment and holding those who perpetrate it responsible for inflicting harm on girls and violating the child or women’s rights (54,68). Some countries have enacted laws against the practice but these laws are usually not enforced (54).
Legislation against FGM/C
The prohibition of FGM/C has been enacted by 26 countries in Africa and the Middle East but the legislation varies from country to country (22). The law in some countries restrict the practice of FGM/C in totality while some restrict the practice in government health facilities and by medical practitioners, for example in Mauritania (22,69). In most African countries legislation against FGM/C involves all age groups while in some non-African countries like United States and Canada the FGM/C is only illegal among minors (22).
The penalties for violating the legislation against FGM/C also vary between countries. While some penalize the circumcisers only, others penalize the circumciser and those that seek for the procedure as an adult or for the minors and some even include anyone who knows that the procedure has been performed and fails to report it (22).
In some African countries, the ban on FGM/C has expanded over the years; for example Kenya expanded its ban to include adult women and extended restrictions to citizens who commit the crime even outside the country’s borders since 2011 (22,70).
Despite all these, FGM/C has not reduced significantly as expected because most of the legislations are not complemented by measures to influence the cultural and religious expectations of the communities within its comprehensive social context (22). Therefore, legislation should be incorporated into strategies to enhance the elimination of FGM/C.
Related practices
While females (particularly when young) are forced by parents, extended family members and their immediate community to undergo FGM/C in developing countries and which practices are globally condemned, individuals in developed countries are voluntarily engaging in practices leading to physical alterations of their body parts and functions. These are piercing, tattooing, enlargement, cosmetic transplantation among others.
Labioplasty, also called “designer vagina” or “vaginal rejuvenation” or “revirgination” is similarly a related practice to FGM/C. This is a genital procedure done to alter the appearance and improve the genital image based on an individual’s satisfaction (68-72). The procedure is carried out in women with absent vaginal passage, intersex conditions, those with physical or psychological discomfort after child birth, advanced age as well as in male-to-female sexual reassignment for the creation of neovagina (71). This is a cosmetic genital surgery done of free will and paid for heavily by clients. When medically indicated for physical or psychological reasons, it is not regarded as FGM/C, but sometimes the procedures are not medically indicated (68,72). The procedure also has similar complications as FGM/C and its safety and effectiveness have not been documented for non-medically indicated reasons (72,73).
Comparison has also been made between male circumcision and FC. Proponents who equate both as being the same argue that they both cause pain and are not medically proven to be beneficial. Those arguing based on their religious beliefs propose that while male circumcision was ordained by the Creator, there is no such documentation of the female variety. Others argue that while male circumcision is done to purify the genitalia, FC is carried out to suppress her sexual urge, a form of discrimination as it were (74).
Acknowledgements
We hereby acknowledge Professor Emiola Oluwabunmi Olapade-Olaopa through whom the invitation to contribute this article was obtained and for his technical advice.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
References
- WHO, Pan American Health Organization (PAHO). Understanding and addressing violence against women. 2012. Accessed on: 18/8/16. Available online: http://www.who.int/reproductivehealth/topics/violence/vaw_series/en/
- Akinsulure-Smith AM, Chu T. Exploring Female Genital Cutting Among Survivors of Torture. J Immigr Minor Health 2017;19:769-73. [Crossref] [PubMed]
- Gruenbaum E. The Female Circumcision Controversy: An Anthropological Perspective. Philadelphia: University of Pennsylvania Press, 2001.
- Teixeira AL, Lisboa M. Estimating the prevalence of female genital mutilation in Portugal. Public Health 2016;139:53-60. [Crossref] [PubMed]
- De Schrijver L, Leye E, Merckx M, et al. A multidisciplinary approach to clitoral reconstruction after female genital mutilation: the crucial role of counselling. Eur J Contracept Reprod Health Care 2016;21:269-75. [Crossref] [PubMed]
- Koukkula M, Keskimäki I, Koponen P, et al. Female Genital Mutilation/Cutting among Women of Somali and Kurdish Origin in Finland. Birth 2016;43:240-6. [Crossref] [PubMed]
- World Health Organization. Female genital mutilation. Fact sheet. Accessed on: July 27, 2016. Available online: http://www.who.int/mediacentre/factsheets/fs241/en/
- United Nations Children’s Fund. Female genital mutilation/cutting: A global concern. 2016. Available online: https://www.unicef.org/media/files/FGMC_2016_brochure_final_UNICEF_SPREAD.pdf
- Inter–African Committee on Traditional Practices (IAC). Accessed on: August 1, 2016. Available online: http://iac-ciaf.net/?view=article&id=18%3Afemale-genital-mutilation-&format=pdf&option=com_content&Itemid=9
- Muteshi JK, Miller S, Belizán JM, et al. The ongoing violence against women: Female Genital Mutilation/Cutting. Reprod Health 2016;13:44. [Crossref] [PubMed]
- Kouba LJ, Muasher J. Female Circumcision in Africa: An Overview. African Studies Review 1985;28:95-110. [Crossref]
- Momoh C. Female Genital Mutilation. Abingdon: Radcliffe Publishing, 2005.
- United Nations Population funds (UNFPA). Female genital mutilation (FGM) frequently asked questions.Accessed on: July 28, 2016. Available online: http://www.unfpa.org/resources/female-genital-mutilation-fgm-frequently-asked-questions#sthash.lLBanQT3.dpuf.
- The Population Council. Survey of young people in Egypt: final report. Cairo, 2005. Accessed on: July 27, 2016. Available online: http://www.popcouncil.org/pdfs/2010PGY_SYPEFinalReport.pdf
- Kandala NB, Nwakeze N, Kandala SN. Spatial distribution of female genital mutilation in Nigeria. Am J Trop Med Hyg 2009;81:784-92. [Crossref] [PubMed]
- National Population Commission and ICF International. Nigeria Demographic and Health Survey, 2013. Abuja, Nigeria, and Rockville, Maryland, USA. 2014. Available online: https://dhsprogram.com/pubs/pdf/FR293/FR293.pdf
- Mpofu S, Odimegwu C, De Wet N, et al. The relation of female circumcision to sexual behavior in Kenya and Nigeria. Women Health 2016.1-18. [Epub ahead of print]. [Crossref] [PubMed]
- Michael Miller M, Moneti F, Lewnes A, et al. Changing a harmful social convention: female genital mutilation/cutting. Florence, Italy: UNICEF Innocenti Research Centre, 2005.
- Wakabi W. Africa battles to make female genital mutilation history. Lancet 2007;369:1069-70. [Crossref] [PubMed]
- Lightfoot-Klein H. The Sexual Experience and Marital Adjustment of Genitally Circumcised and Infibulated Females in the Sudan. The Journal of Sex Research 1989;26:375-92. [Crossref]
- Lightfoot-Klein H. Prisoners of Ritual: An Odyssey into Female Genital Circumcision in Africa. New York: Routledge, 1989.
- United Nations Children’s Fund. Female Genital Mutilation/Cutting: A statistical overview and exploration of the dynamics of change. 2013. Accessed on: July 27, 2016. Available online: http://www.unicef.org/media/files/FGCM_Lo_res.pdf
- El Dareer A. Woman, Why Do You Weep? Circumcision and Its Consequences. London: Zed Press, 1983:56-64.
- Balogun OO, Hirayama F, Wariki WM, et al. Interventions for improving outcomes for pregnant women who have experienced genital cutting. Cochrane Database Syst Rev 2013.CD009872. [PubMed]
- Dorkenoo E, Elworthy S. Female genital mutilation: proposals for change. London Minority Rights Group 1992;11-5:30-5.
- Gruenbaum E. Socio-cultural dynamics of female genital cutting: research findings, gaps, and directions. Cult Health Sex 2005;7:429-41. [Crossref] [PubMed]
- Serour GI. Medicalization of female genital mutilation/cutting. Afr J Urol 2013;19:145-9. [Crossref]
- Kaplan A, Hechavarría S, Martín M, et al. Health consequences of female genital mutilation/cutting in the Gambia, evidence into action. Reprod Health 2011;8:26. [Crossref] [PubMed]
- Bishai D, Bonnenfant YT, Darwish M, et al. Estimating the obstetric costs of female genital mutilation in six African countries. Bull World Health Organ 2010;88:281-8. [Crossref] [PubMed]
- Berg RC, Underland V, Odgaard-Jensen J, et al. Effects of female genital cutting on physical health outcomes: a systematic review and meta-analysis. BMJ Open 2014;4:e006316. [Crossref] [PubMed]
- Adekunle AO, Fakokunde FA, Odukogbe AA, et al. Female genital mutilation - postcircumcision vulval complications in Nigerians. J Obstet Gynaecol 1999;19:632-5. [Crossref] [PubMed]
- WHO study group on female genital mutilation and obstetric outcome, Banks E, Meirik O, et al. Female genital mutilation and obstetric outcome: WHO collaborative prospective study in six African countries. Lancet 2006;367:1835-41.
- Vital M, de Visme S, Hanf M, et al. Using the Female Sexual Function Index (FSFI) to evaluate sexual function in women with genital mutilation undergoing surgical reconstruction: a pilot prospective study. Eur J Obstet Gynecol Reprod Biol 2016;202:71-4. [Crossref] [PubMed]
- Mitchell M. FGM and midwifery practice. Pract Midwife 2016;19:13-6. [PubMed]
- Momoh C, Olufade O, Redman-Pinard P. What nurses need to know about female genital mutilation. Br J Nurs 2016;25:S30-4. [Crossref] [PubMed]
- RCN calls for improved information sharing on FGM. Nurs Stand 2016;30:11. [PubMed]
- Nowak B. The School Nurse's Role in Addressing Female Genital Mutilation. NASN Sch Nurse 2016;31:286-91. [Crossref] [PubMed]
- Abramowicz S, Oden S, Dietrich G, et al. Anatomic, functional and identity results after clitoris transposition. J Gynecol Obstet Biol Reprod (Paris) 2016;45:963-971. [Crossref] [PubMed]
- Abdulcadir J, McLaren S, Boulvain M, et al. Health education and clinical care of immigrant women with female genital mutilation/cutting who request postpartum reinfibulation. Int J Gynaecol Obstet 2016;135:69-72. [Crossref] [PubMed]
- Abdel-Azim S. Psychosocial and sexual aspects of female circumcision. Afr J Urol 2013;19:141-2. [Crossref]
- Balon R. Sexual dysfunction, the brain–body connection. Basel: Adv Psychosom Med Basel, 2008.
- Berg RC, Denison E. Does Female Genital Mutilation/Cutting (FGM/C) Affect Women’s Sexual Functioning? A Systematic Review of the Sexual Consequences of FGM/C. Sex Res Social Policy 2012;9:41-56. [Crossref]
- el-Defrawi MH, Lotfy G, Dandash KF, et al. Female genital mutilation and its psychosexual impact. J Sex Marital Ther 2001;27:465-73. [Crossref] [PubMed]
- Hassanin IM, Helmy YA, Fathalla MM, et al. Prevalence and characteristics of female sexual dysfunction in a sample of women from Upper Egypt. Int J Gynaecol Obstet 2010;108:219-23. [Crossref] [PubMed]
- Rushwan H. Female genital mutilation: A tragedy for women's reproductive health. Afr J Urol 2013;19:130-3. [Crossref]
- Yamamiya Y, Cash TF, Thompson JK. Sexual Experiences among College Women: The Differential Effects of General versus Contextual Body Images on Sexuality. Sex Roles 2006;55:421-7. [Crossref]
- Herbenick D, Schick V, Reece M, et al. The Female Genital Self-Image Scale (FGSIS): results from a nationally representative probability sample of women in the United States. J Sex Med 2011;8:158-66. [Crossref] [PubMed]
- Krause E, Brandner S, Mueller MD, et al. Out of Eastern Africa: defibulation and sexual function in woman with female genital mutilation. J Sex Med 2011;8:1420-5. [Crossref] [PubMed]
- Berg RC, Denison E, Fretheim A. Psychological, social and sexual consequences of female genital mutilation/cutting (FGM/C): a systematic review of quantitative studies. Report from Kunnskapssenteret nr 13−2010. Oslo: Nasjonalt kunnskapssenter for helsetjenesten, 2010. Accessed on: Aug 20, 2016. Available online: hera.helsebiblioteket.no/hera/bitstream/10143/132233/1/NOKCrapport13_2010.pdf
- MacLeod T. Female genital mutilation. J Soc Gynaecol Can 1995;17:333-42.
- World Health Organization (WHO). Health risks of female genital mutilation (FGM). Accessed on: 20/8/16. Available online: www.who.int/reproductivehealth/topics/fgm/health_consequences_fgm/en/
- Heiman J. Orgasmic disorders in women. In: Leiblum S. editor. Principles and practice of sex therapy. 4th edition. New York: The Guilford Press, 2007:84-123.
- Meniru GI. Female genital mutilation (female circumcision). Br J Obstet Gynaecol 1994;101:832. [Crossref] [PubMed]
- Nour NM. Female genital cutting: a persisting practice. Rev Obstet Gynecol 2008;1:135-9. [PubMed]
- Sharfi AR, Elmegboul MA, Abdella AA. The continuing challenge of female genital mutilation in Sudan. Afr J Urol 2013;19:136-40. [Crossref]
- Baasher T. Psychological aspects of female circumcision in traditional practice affecting the health of woman; 1979. Report of a seminar WHO/EMRO Publication, No. 2. Alexandria, 1979.
- Larsen U, Okonofua FE. Female circumcision and obstetric complications. Int J Gynaecol Obstet 2002;77:255-65. [Crossref] [PubMed]
- Johnson EB, Reed SD, Hitti J, et al. Increased risk of adverse pregnancy outcome among Somali immigrants in Washington state. Am J Obstet Gynecol 2005;193:475-82. [Crossref] [PubMed]
- Rouzi AA, Aljhadali EA, Amarin ZO, et al. The use of intrapartum defibulation in women with female genital mutilation. BJOG 2001;108:949-51. [Crossref] [PubMed]
- Kaplan A, Forbes M, Bonhoure I, et al. Female genital mutilation/cutting in The Gambia: long-term health consequences and complications during delivery and for the newborn. Int J Womens Health 2013;5:323-31. [Crossref] [PubMed]
- Browning A, Allsworth JE, Wall LL. The relationship between female genital cutting and obstetric fistulae. Obstet Gynecol 2010;115:578-83. [Crossref] [PubMed]
- Yasin BA, Al-Tawil NG, Shabila NP, et al. Female genital mutilation among Iraqi Kurdish women: a cross-sectional study from Erbil city. BMC Public Health 2013;13:809. [Crossref] [PubMed]
- Jiménez-Ruiz I, Almansa Martínez P, Pastor Bravo Mdel M. Male perceptions of sequelae associated with female genital mutilation. Gac Sanit 2016;30:258-64. [PubMed]
- Achia TN. Spatial modelling and mapping of female genital mutilation in Kenya. BMC Public Health 2014;14:276. [Crossref] [PubMed]
- Yount KM. Like mother, like daughter? Female genital cutting in Minia, Egypt. J Health Soc Behav 2002;43:336-58. [Crossref] [PubMed]
- Ministry of Health and Population [Egypt], El-Zanaty and Associates [Egypt], and ICF International. Egypt Demographic and Health Survey 2014. Cairo, Egypt and Rockville, Maryland, USA. 2015. Accessed on: July 29, 2016. Available online: dhsprogram.com/pubs/pdf/fr302/fr302.pdf.
- Modrek S, Liu JX. Exploration of pathways related to the decline in female circumcision in Egypt. BMC Public Health 2013;13:921. [Crossref] [PubMed]
- World Health Organization (WHO). Eliminating female genital mutilation. 2008. Accessed on: Aug 21, 16. Available at: www.who.int/reproductivehealth/publications/fgm/9789241596442/en/
- UNICEF. Legislative Reform to Support the Abandonment of Female Genital Mutilation/Cutting. Available online: https://www.unicef.org/policyanalysis/files/UNICEF_-_LRI_Legislative_Reform_to_support_the_Abandonment_of_FGMC_August_2010.pdf
- National Council for Law Reporting. Prohibition of Female Genital Mutilation Act. 2011. Accessed on: Aug 21, 16. Available online: http://www.kenyalaw.org/klr/fileadmin/pdfdownloads/Acts/ProhibitionofFemaleGenitalMutilationAct_No32of2011.pdf
- Lloyd J, Crouch NS, Minto CL, et al. Female genital appearance: "normality" unfolds. BJOG 2005;112:643-6. [Crossref] [PubMed]
- American Congress of Obstetricians and Gynecologists (ACOG). ACOG Advises Against Cosmetic Vaginal Procedures Due to Lack of Safety and Efficacy Data. Available online: http://www.acog.org/About-ACOG/News-Room/News-Releases/2007/ACOG-Advises-Against-Cosmetic-Vaginal-Procedures
- Committee on Gynecologic Practice, American College of Obstetricians and Gynecologists. ACOG Committee Opinion No. 378: Vaginal "rejuvenation" and cosmetic vaginal procedures. Obstet Gynecol 2007;110:737-8. [Crossref] [PubMed]
- Mcalister RD. A dangerous muddying of the waters? The 'significant harm' of re B and G (children) (care proceedings)[2015] EWFC 3. Med Law Rev 2016;24:259-67. [Crossref] [PubMed]


