Premature ejaculation: do we have effective therapy?
Introduction
Ejaculatory dysfunction (EjD), erectile dysfunction (ED) and premature ejaculation (PE) are the three main subtypes of male sexual dysfunction (1). It has been more than a century since the initial report regarding PE was published (2), but the definition, classification, prevalence and effective treatment options for PE are still under debate (3). Although PE is classically accepted to be the most common sexual dysfunction (4-8), the number of PE patients who seek treatment for this condition is low (8,9). Hence, almost 75% of urologists in the U.S. reported seeing less than one PE patient per week (10), and 41.4% of European urology residents denied treating any PE patients (11). Lack of exposure to patients with PE during urology residency training results in a lack of knowledge regarding the principal clinical guidelines for the treatment of PE (11). This highlights a need for increased awareness and education of available, effective management options.
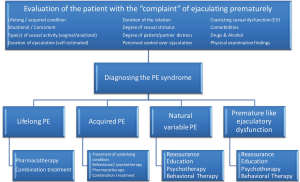
Historically, treatments for PE were limited to psychological and behavioral therapies; however, more recent reports include pharmacotherapy as a common first-line treatment (Table 1) (10). To date, the U.S. Food and Drug Administration (FDA) has not approved any medications for the primary treatment of PE. As such, any medical treatments are currently administered off-label, and patients must therefore be counseled as to the risks and benefits of therapy. Treatments must additionally be individualized according to the type of PE complaint, as well as patient and partner preferences (Figure 1).
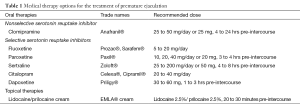
Full table
Psychological/behavioral strategies
Although effective pharmacologic treatments have reduced the popularity of traditional, psychological/behavioral therapies, these methods remain a mainstay treatment in patients with natural, variable PE and premature-like EjD (9,12). In addition, providing basic psychosexual education and therapy to all patients seeking treatment for PE may be of benefit, as PE results in reduced sexual satisfaction and function along with increased levels of personal distress and interpersonal difficulty (13).
Although pharmacotherapy is superior in reducing PE symptoms when compared to psychological treatment alone, behavioral and psychologic therapies offer potential advantages including minimal side effects and ability to improve couples’ sexual communication. These therapies may also be used alone or in combination with pharmacotherapy among patients with lifelong and acquired PE (14-16). On the other hand, psychotherapeutic approaches are time-consuming, costly (17,18), and are of variable efficacy (19). Because of a paucity of well-controlled studies and well-defined treatment protocols there is an overall lack of evidence suggesting beneficial effects of psychotherapy on PE (20,21).
Commonly utilized behavioral methods include the ‘stop-start’ technique, first developed by Semans (22) and its modification, the ‘squeeze’ method, proposed by Masters and Johnson (23). These methods inhibit the urge to ejaculate by attenuating sexual stimulus. Masturbation prior to sexual intercourse is widely used by younger men and it has similar efficacy to the ‘start-stop’ technique (24-26). Another related therapy is pelvic floor rehabilitation exercises, with a recent small, randomized prospective study reporting similar efficacy to on demand dapoxetine in the treatment of lifelong PE (27,28). Overall, behavioral therapies result in success rates of 50-60% in the short term, with significantly reduced efficacy with additional follow-up (17,18). However, the combination of behavioral and pharmacotherapy may result in synergistic improvements, with additional studies required to further elucidate potential beneficial effects (29).
Pharmacotherapy
Topical agents
Topical anesthetic compounds were the first medical treatment proposed for PE (30). Lidocaine-prilocaine creams decrease the sensation of the penis and significantly increase intravaginal ejaculatory latency time (IELT) when applied 10 to 20 minutes prior to sexual activity (31-33). This benefit is further enhanced when lidocaine-prilocaine cream is combined with sildenafil (34). A topical lidocaine-prilocaine-containing spray has recently been developed (topical eutectic mixture for premature ejaculation; TEMPE Plethora Solutions Ltd, London, UK), with initial results demonstrating a 6.3-fold increase of IELT and an associated improvement in patient reported outcome (PRO) measures of control and sexual satisfaction (35). As the topical aerosol has minimal local and negligible systemic side effects, it will likely receive appropriate regulatory approval for the treatment of PE in the near future (36). Another topical anesthetic agent available in Korea is SS-cream, a solution that is made from the extracts of nine different herbs (37). In a double-blind, randomized, placebo-controlled study, 82% of patients reported improved sexual satisfaction with mean IELT increase from 1.37 to 10.92 min (38).
Side effects of topical agents include penile hypoesthesia, transvaginal absorption resulting in vaginal numbness, penile/vaginal dermatitis, and difficulties in product application (33,39). However, given the overall efficacy and limited side effects, current PE guidelines recommend topical therapy as a viable treatment option for the management of PE (14,40).
Oral therapies
The quest of finding an oral treatment for PE dates back to 1943 (30). Initial agents to prolong coitus were alpha amino benzoate and phenoxybenzamine, both of which were associated with severe side effects (41-44). Tricyclic antidepressants and ultimately selective serotonin reuptake inhibitors (SSRIs) were subsequently utilized, due to their sustained efficacy on ejaculatory latency and tolerable side effect profile (45-50). The mechanism for delayed ejaculation with SSRIs likely relates to the inhibition of multiple descending pathways associated with the ejaculatory reflex (51). This is supported by studies demonstrating significant variations in cortical serotonergic function between patients with PE and normal volunteers (52).
SSRIs interact with the 5-HT2C receptor causing a delay in ejaculation (53,54). Results may become evident within a few days of treatment onset; however, maximal improvements are usually not evident until 2 to 3 weeks of treatment (55-58). The therapeutic efficacy of daily SSRIs on PE are supported by multiple, double-blind, placebo-controlled trials (59). Thus, guidelines for lifelong PE often recommend oral SSRIs as first line medical therapy (14,39). Among the available SSRIs, paroxetine has demonstrated greater benefits in regards to efficacy and side effects when compared to fluoxetine, clomipramine and sertraline (60,61).
In addition to known systemic effects, SSRIs are associated with sexual side effects including decreased fertility and ED. Chronic SSRI treatment has a detrimental effect on spermatogenesis, impairs sperm transport, damages the sperm cell membrane, alters sperm DNA and has various effects on hormonal homeostasis (62-66). Given these findings, patients desiring preserved fertility should be considered for alternative therapies to prevent potential impaired spermatogenesis (62-66).
A number of animal studies have demonstrated that SSRIs may not only affect fertility, but also impair erectile function. Angulo et al. (67) hypothesize that decreased erectile function with paroxetine is secondary to reduced nitric oxide (NO) production and neuronal nitric oxide synthase (nNOS) expression. Kadioglu et al. suggested that sertraline and fluoxetine result in dysregulation of various relaxing factors, most conceivably NO, while paroxetine contributes to erectile dysfunction via different NOS inhibitory activity (68). Unwanted sexual side effects, such as decreased libido, anorgasmia, and erectile dysfunction are limitations associated with serotonergic antidepressants, which may persist beyond cessation of SSRI treatment (69,70).
Dapoxetine is a more recently developed SSRI that is quickly absorbed and rapidly cleared from the body (71). In contrast to other SSRIs, it may be used in an on-demand fashion, given its rapid onset of action. Recent trials with dapoxetine have demonstrated an increase in IELT by a factor of 2.5 to 3 over baseline (36). A recent analysis of five phase III trials of dapoxetine demonstrated that at 12 weeks of treatment the average IELT increased from a baseline of 0.9 to 3.1 minutes with 30 mg dapoxetine and to 3.6 minutes with 60 mg versus an increase to 1.9 minutes with placebo (72,73). Men with lifelong and acquired PE have reported efficacy with dapoxetine (74). Dapoxetine has not been reported to have any drug–drug interactions, including with PDE-5 inhibitors (75); however, dapoxetine has been rarely associated with vasovagal-mediated syncope (76). Although on-demand treatment provides a convenient therapy, a study performed by Waldinger and Schweitzer among lifelong PE patients demonstrated preference for daily over on-demand therapy, as this guaranteed no interference with the spontaneity of sexual activity (77). The data published on dapoxetine remains a hot topic, given the dynamic nature of the PE drug research field (78).
Another potential treatment option for PE is PDE-5 inhibitors. In one randomized, double-blind, placebo-controlled study involving sildenafil in men with PE, there was no significant change in IELT, however, there was evidence of increased confidence, perception of ejaculatory control, overall sexual satisfaction, and decreased refractory time to achieve a second erection after ejaculation (79). Another randomized, double-blind, placebo-controlled study with sildenafil found the efficacy similar to that of placebo (34). In contrast, other randomized, double-blind, parallel group studies with sildenafil showed significantly improved IELT and satisfaction, with reduced overall anxiety compared to several SSRIs and behavioral therapy (80,81).
Available data on alternative PDE-5 inhibitors, tadalafil and vardenafil, is currently limited (80,81). One report found that vardenafil significantly increased median ejaculatory latency time duration during vibratory stimulation compared to placebo, while both sildenafil and tadalafil showed no significant change (82). In men who have acquired PE with comorbid ED, a PDE-5 inhibitor alone or in combination with a SSRI may provide benefit (83). PDE-5 as monotherapy or as a component of a combination regimen was similarly supported by another recent meta-analysis, that showed an overall positive effect with use in the treatment of PE (84). The use of PDE-5 inhibitors for the treatment of PE will likely continue to increase, as the association between NO and PE is further clarified (85).
Another novel approach postulated to decrease PE is the use of alpha-1 adrenergic antagonists, such as terazosin and alfuzosin (86,87). A recent small study including eight patients who were given alpha-1 adrenergic antagonist monotherapy for PE found that IELT was significantly prolonged from 3.4 to 10.1 minutes (P=0.003). All patients felt their PE problem was better controlled when compared with their pretreatment condition (88). These results support further randomized controlled trials to uncover the true efficacy of alpha-1 adrenergic antagonists in PE management.
Opioid analgesics, most specifically tramadol, have proven to be effective for on-demand treatment of PE in several placebo-controlled studies. In two trials, tramadol 50 mg increased IELT, measures of sexual satisfaction, and the sense of ejaculatory control (89,90). Another trial administering 25 mg of tramadol, as needed, increased IELT from a baseline of 1.17 to 7.37 minutes after treatment (90). A subsequent single-blinded, randomized, controlled trial of 60 patients further confirmed the efficacy of on-demand tramadol (91). Most recently, a multicenter double-blind, placebo-controlled trial of tramadol 62 mg orally disintegrating tablet (ODT) preparation involving 600 patients from 62 sites across 11 countries found significant improvement in IELT, with minimal adverse effects or tolerability issues reported (92). In a subgroup of over 300 men with a baseline IELT <1 minute, results were even more pronounced, with a 2.4-fold increase in IELT observed with 62 mg tramadol ODT (92). Inversely, patients complaining of delayed ejaculation who subsequently discontinue tramadol therapy have reported improvements in sexual function, although the underlying mechanism is not completely understood (93). Given potential long-term effects of tramadol therapy, further studies are needed to determine the risk of drug dependence and potential interactions with combined therapies, including PDE-5 inhibitors (94).
Several less conventional methods have been investigated for the treatment of PE. Sunay et al. demonstrated that acupuncture had a significant effect in delaying ejaculation when compared to placebo, although results were inferior to daily paroxetine (95). Additional studies further support the role of acupuncture in the management of PE (96).
Miscellaneous treatments
Surgical therapy is an additional option described for the management of select, refractory cases of PE. Surgically induced penile hypoanesthesia via selective dorsal nerve neurotomy or hyaluronic acid gel glans penis augmentation has been reported by several authors for the treatment of lifelong PE, which is otherwise unresponsive to behavioral and pharmacological treatment (97,98). In one recently published study, surgical foreskin remnant removal resulted in significant increases in IELT, from a baseline of 64.25 seconds before surgery to 731.49 seconds following (99). Further studies are required to better understand the role of surgical management of PE, although most authorities indicate that surgical management is not indicated and should be avoided (14).
As the underlying etiology for PE is frequently multifactorial, management of PE patients can be complex and may require a combination of treatment modalities (100). The physician must consider the severity of symptoms and potential side effects of various therapies when deciding on how to treat a PE patient. A combination of pharmacological, psychological, and behavioral approaches for the man with PE should be utilized in clinical practice, and when possible, the partner should be included in management (101). Successful treatment of PE patients requires ongoing follow-up to help monitor for improvement and ensure optimal treatment outcomes (102). An all-encompassing and more structured diagnostic approach to PE will help clinicians develop a greater understanding of PE and lead to better treatment outcomes in the future (103).
Conclusions
Data from recent studies has improved understanding of the underlying mechanism for PE and provided evidence-based management options. Further investigations with randomized-controlled trials, using a consistent definition of PE are needed. Currently, clinicians need to consider all treatment modalities when evaluating a man with PE, as each patient may respond differently and experience variable side effects. As our understanding of the mechanism of PE increases, additional and more effective therapies will continue to be developed.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
References
- Rosen RC, McMahon CG, Niederberger C, et al. Correlates to the clinical diagnosis of premature ejaculation: results from a large observational study of men and their partners. J Urol 2007;177:1059-64. [PubMed]
- Gross S. eds. Practical treatise on impotence and sterility and allied disorders of the male sexual organs. Edinburg: YJ Pentland; 1887.
- Serefoglu EC, Saitz TR. New insights on premature ejaculation: a review of definition, classification, prevalence and treatment. Asian J Androl 2012;14:822-9. [PubMed]
- Aschka C, Himmel W, Ittner E, et al. Sexual problems of male patients in family practice. J Fam Pract 2001;50:773-8. [PubMed]
- Laumann EO, Paik A, Rosen RC. Sexual dysfunction in the United States: prevalence and predictors. JAMA 1999;281:537-44. [PubMed]
- Simons JS, Carey MP. Prevalence of sexual dysfunctions: results from a decade of research. Arch Sex Behav 2001;30:177-219. [PubMed]
- Frank E, Anderson C, Rubinstein D. Frequency of sexual dysfunction in “normal” couples. N Engl J Med 1978;299:111-5. [PubMed]
- Serefoglu EC, Yaman O, Cayan S, et al. Prevalence of the complaint of ejaculating prematurely and the four premature ejaculation syndromes: results from the Turkish Society of Andrology Sexual Health Survey. J Sex Med 2011;8:540-8. [PubMed]
- Waldinger MD. Premature ejaculation: state of the art. Urol Clin North Am 2007;34:591-9. vii-viii. [PubMed]
- Shindel A, Nelson C, Brandes S. Urologist practice patterns in the management of premature ejaculation: a nationwide survey. J Sex Med 2008;5:199-205. [PubMed]
- Luján S, García-Fadrique G, Morales G, et al. Are urology residents ready to treat premature ejaculation after their training? J Sex Med 2012;9:404-10. [PubMed]
- Waldinger MD. Recent advances in the classification, neurobiology and treatment of premature ejaculation. Adv Psychosom Med 2008;29:50-69. [PubMed]
- Rowland DL, Patrick DL, Rothman M, et al. The psychological burden of premature ejaculation. J Urol 2007;177:1065-70. [PubMed]
- Althof SE, Abdo CH, Dean J, et al. International Society for Sexual Medicine's guidelines for the diagnosis and treatment of premature ejaculation. J Sex Med 2010;7:2947-69. [PubMed]
- Rowland D, Cooper S. Practical tips for sexual counseling and psychotherapy in premature ejaculation. J Sex Med 2011;8:342-52. [PubMed]
- Hartmann UH. Words of Wisdom. Re: combination therapy for premature ejaculation: results of a small-scale study. Eur Urol 2011;59:169-71. [PubMed]
- Hawton K, Catalan J, Martin P, et al. Long-term outcome of sex therapy. Behav Res Ther 1986;24:665-75. [PubMed]
- De Amicis LA, Goldberg DC, LoPiccolo J, et al. Clinical follow-up of couples treated for sexual dysfunction. Arch Sex Behav 1985;14:467-89. [PubMed]
- Melnik T, Althof S, Atallah AN, et al. Psychosocial interventions for premature ejaculation. Cochrane Database Syst Rev 2011.CD008195. [PubMed]
- Althof SE. Psychological treatment strategies for rapid ejaculation: rationale, practical aspects, and outcome. World J Urol 2005;23:89-92. [PubMed]
- Heiman JR, Meston CM. Empirically validated treatment for sexual dysfunction. Annu Rev Sex Res 1997;8:148-94. [PubMed]
- Semans JH. Premature ejaculation: a new approach. South Med J 1956;49:353-8. [PubMed]
- Masters WH, Johnson VE. eds. Human sexual inadequacy. Boston: Little & Brown, 1970.
- de Carufel F, Trudel G. Effects of a new functional-sexological treatment for premature ejaculation. J Sex Marital Ther 2006;32:97-114. [PubMed]
- Grenier G, Byers ES. Rapid ejaculation: a review of conceptual, etiological, and treatment issues. Arch Sex Behav 1995;24:447-72. [PubMed]
- Metz ME, Pryor JL, Nesvacil LJ, et al. Premature ejaculation: a psychophysiological review. J Sex Marital Ther 1997;23:3-23. [PubMed]
- Pastore AL, Palleschi G, Leto A, et al. A prospective randomized study to compare pelvic floor rehabilitation and dapoxetine for treatment of lifelong premature ejaculation. Int J Androl 2012;35:528-33. [PubMed]
- La Pera G, Nicastro A. A new treatment for premature ejaculation: the rehabilitation of the pelvic floor. J Sex Marital Ther 1996;22:22-6. [PubMed]
- Hartmann UH. Words of wisdom. Re: Effects of a new functional-sexological treatment for premature ejaculation. Eur Urol 2007;52:1259-61. [PubMed]
- Schapiro B. Premature ejaculation: a review of 1130 cases. J Urol 1943;50:374-9.
- Atikeler MK, Gecit I, Senol FA. Optimum usage of prilocaine-lidocaine cream in premature ejaculation. Andrologia 2002;34:356-9. [PubMed]
- Berkovitch M, Keresteci AG, Koren G. Efficacy of prilocaine-lidocaine cream in the treatment of premature ejaculation. J Urol 1995;154:1360-1. [PubMed]
- Busato W, Galindo CC. Topical anaesthetic use for treating premature ejaculation: a double-blind, randomized, placebo-controlled study. BJU Int 2004;93:1018-21. [PubMed]
- Atan A, Basar MM, Tuncel A, et al. Comparison of efficacy of sildenafil-only, sildenafil plus topical EMLA cream, and topical EMLA-cream-only in treatment of premature ejaculation. Urology 2006;67:388-91. [PubMed]
- Dinsmore WW, Hackett G, Goldmeier D, et al. Topical eutectic mixture for premature ejaculation (TEMPE): a novel aerosol-delivery form of lidocaine-prilocaine for treating premature ejaculation. BJU Int 2007;99:369-75. [PubMed]
- Mohee A, Eardley I. Medical therapy for premature ejaculation. Ther Adv Urol 2011;3:211-22. [PubMed]
- Morales A, Barada J, Wyllie MG. A review of the current status of topical treatments for premature ejaculation. BJU Int 2007;100:493-501. [PubMed]
- Choi HK, Jung GW, Moon KH, et al. Clinical study of SS-cream in patients with lifelong premature ejaculation. Urology 2000;55:257-61. [PubMed]
- Sadeghi-Nejad H, Watson R. Premature ejaculation: current medical treatment and new directions (CME). J Sex Med 2008;5:1037-50. [PubMed]
- Hatzimouratidis K, Amar E, Eardley I, et al. Guidelines on male sexual dysfunction: erectile dysfunction and premature ejaculation. Eur Urol 2010;57:804-14. [PubMed]
- Aycock L. The medical management of premature ejaculation. J Urol 1949;62:361. [PubMed]
- Damrau F. Premature ejaculation: use of ethyl aminobenzoate to prolong coitus. J Urol 1963;89:936-9. [PubMed]
- Shilon M, Paz GF, Homonnai ZT. The use of phenoxybenzamine treatment in premature ejaculation. Fertil Steril 1984;42:659-61. [PubMed]
- Beretta G, Chelo E, Fanciullacci F, et al. Effect of an alpha-blocking agent (phenoxybenzamine) in the management of premature ejaculation. Acta Eur Fertil 1986;17:43-5. [PubMed]
- Rowland DL, De Gouveia Brazao CA, Koos Slob A. Effective daily treatment with clomipramine in men with premature ejaculation when 25 mg (as required) is ineffective. BJU Int 2001;87:357-60. [PubMed]
- Strassberg DS, de Gouveia Brazao CA, Rowland DL, et al. Clomipramine in the treatment of rapid (premature) ejaculation. J Sex Marital Ther 1999;25:89-101. [PubMed]
- Assalian P. Clomipramine in the treatment of premature ejaculation. J Sex Res 1988;24:213-5. [PubMed]
- Segraves RT, Saran A, Segraves K, et al. Clomipramine versus placebo in the treatment of premature ejaculation: a pilot study. J Sex Marital Ther 1993;19:198-200. [PubMed]
- Goodman RE. An assessment of clomipramine (Anafranil) in the treatment of premature ejaculation. J Int Med Res 1980;8:53-9. [PubMed]
- Waldinger MD, Zwinderman AH, Olivier B. On-demand treatment of premature ejaculation with clomipramine and paroxetine: a randomized, double-blind fixed-dose study with stopwatch assessment. Eur Urol 2004;46:510-5. [PubMed]
- Giuliano F, Clément P. Serotonin and premature ejaculation: from physiology to patient management. Eur Urol 2006;50:454-66. [PubMed]
- Kwon OY, Kam SC, Choi JH, et al. Effects of sertraline on brain current source of the high beta frequency band: analysis of electroencephalography during audiovisual erotic stimulation in males with premature ejaculation. Int J Impot Res 2011;23:213-9. [PubMed]
- Patterson WM. Fluoxetine-induced sexual dysfunction. J Clin Psychiatry 1993;54:71. [PubMed]
- Forster P, King J. Fluoxetine for premature ejaculation. Am J Psychiatry 1994;151:1523. [PubMed]
- Giuliano F. 5-Hydroxytryptamine in premature ejaculation: opportunities for therapeutic intervention. Trends Neurosci 2007;30:79-84. [PubMed]
- Waldinger MD. Premature ejaculation: definition and drug treatment. Drugs 2007;67:547-68. [PubMed]
- Waldinger MD. Lifelong premature ejaculation: definition, serotonergic neurotransmission and drug treatment. World J Urol 2005;23:102-8. [PubMed]
- Giuliano F. Premature ejaculation: definition and drug treatment. Drugs 2007;67:1629-30. [PubMed]
- Waldinger MD, Zwinderman AH, Schweitzer DH, et al. Relevance of methodological design for the interpretation of efficacy of drug treatment of premature ejaculation: a systematic review and meta-analysis. Int J Impot Res 2004;16:369-81. [PubMed]
- Waldinger MD, Zwinderman AH, Olivier B. SSRIs and ejaculation: a double-blind, randomized, fixed-dose study with paroxetine and citalopram. J Clin Psychopharmacol 2001;21:556-60. [PubMed]
- Waldinger MD, Hengeveld MW, Zwinderman AH, et al. Effect of SSRI antidepressants on ejaculation: a double-blind, randomized, placebo-controlled study with fluoxetine, fluvoxamine, paroxetine, and sertraline. J Clin Psychopharmacol 1998;18:274-81. [PubMed]
- Koyuncu H, Serefoglu EC, Ozdemir AT, et al. Deleterious effects of selective serotonin reuptake inhibitor treatment on semen parameters in patients with lifelong premature ejaculation. Int J Impot Res 2012;24:171-3. [PubMed]
- Koyuncu H, Serefoglu EC, Yencilek E, et al. Escitalopram treatment for premature ejaculation has a negative effect on semen parameters. Int J Impot Res 2011;23:257-61. [PubMed]
- Tanrikut C, Feldman AS, Altemus M, et al. Adverse effect of paroxetine on sperm. Fertil Steril 2010;94:1021-6. [PubMed]
- Tanrikut C, Schlegel PN. Antidepressant-associated changes in semen parameters. Urology 2007;69:185.e5-7.
- Safarinejad MR. Sperm DNA damage and semen quality impairment after treatment with selective serotonin reuptake inhibitors detected using semen analysis and sperm chromatin structure assay. J Urol 2008;180:2124-8. [PubMed]
- Angulo J, Peiró C, Sanchez-Ferrer CF, et al. Differential effects of serotonin reuptake inhibitors on erectile responses, NO-production, and neuronal NO synthase expression in rat corpus cavernosum tissue. Br J Pharmacol 2001;134:1190-4. [PubMed]
- Kadioglu M, Muci E, Ozyavuz R, et al. Paroxetine inhibited the relaxations induced by EFS in mice corpus cavernosum: is it a NOS inhibition? Fundam Clin Pharmacol 2010;24:55-61. [PubMed]
- Bolton JM, Sareen J, Reiss JP. Genital anaesthesia persisting six years after sertraline discontinuation. J Sex Marital Ther 2006;32:327-30. [PubMed]
- Csoka AB, Bahrick A, Mehtonen OP. Persistent sexual dysfunction after discontinuation of selective serotonin reuptake inhibitors. J Sex Med 2008;5:227-33. [PubMed]
- Pryor JL, Althof SE, Steidle C, et al. Efficacy and tolerability of dapoxetine in treatment of premature ejaculation: an integrated analysis of two double-blind, randomised controlled trials. Lancet 2006;368:929-37. [PubMed]
- McMahon CG, Althof SE, Kaufman JM, et al. Efficacy and safety of dapoxetine for the treatment of premature ejaculation: integrated analysis of results from five phase 3 trials. J Sex Med 2011;8:524-39. [PubMed]
- Buvat J, Tesfaye F, Rothman M, et al. Dapoxetine for the treatment of premature ejaculation: results from a randomized, double-blind, placebo-controlled phase 3 trial in 22 countries. Eur Urol 2009;55:957-67. [PubMed]
- Porst H, McMahon CG, Althof SE, et al. Baseline characteristics and treatment outcomes for men with acquired or lifelong premature ejaculation with mild or no erectile dysfunction: integrated analyses of two phase 3 dapoxetine trials. J Sex Med 2010;7:2231-42. [PubMed]
- Dresser MJ, Desai D, Gidwani S, et al. Dapoxetine, a novel treatment for premature ejaculation, does not have pharmacokinetic interactions with phosphodiesterase-5 inhibitors. Int J Impot Res 2006;18:104-10. [PubMed]
- Hutchinson K, Cruickshank K, Wylie K. A benefit-risk assessment of dapoxetine in the treatment of premature ejaculation. Drug Saf 2012;35:359-72. [PubMed]
- Waldinger MD, Zwinderman AH, Olivier B, et al. The majority of men with lifelong premature ejaculation prefer daily drug treatment: an observation study in a consecutive group of Dutch men. J Sex Med 2007;4:1028-37. [PubMed]
- Waldinger MD, Schweitzer DH. Premature ejaculation and pharmaceutical company-based medicine: the dapoxetine case. J Sex Med 2008;5:966-97. [PubMed]
- McMahon CG, Stuckey BG, Andersen M, et al. Efficacy of sildenafil citrate (Viagra) in men with premature ejaculation. J Sex Med 2005;2:368-75. [PubMed]
- McMahon CG, McMahon CN, Leow LJ, et al. Efficacy of type-5 phosphodiesterase inhibitors in the drug treatment of premature ejaculation: a systematic review. BJU Int 2006;98:259-72. [PubMed]
- Wang WF, Minhas S, Ralph DJ. Phosphodiesterase 5 inhibitors in the treatment of premature ejaculation. Int J Androl 2006;29:503-09. [PubMed]
- Gökçe A, Halis F, Demirtas A, et al. The effects of three phosphodiesterase type 5 inhibitors on ejaculation latency time in lifelong premature ejaculators: a double-blind laboratory setting study. BJU Int 2011;107:1274-7. [PubMed]
- Sommer F, Klotz T, Mathers MJ. Treatment of premature ejaculation: A comparative vardenafil and SSRI crossover study. J Urol 2005;174:202.
- Asimakopoulos AD, Miano R, Finazzi Agrò E, et al. Does current scientific and clinical evidence support the use of phosphodiesterase type 5 inhibitors for the treatment of premature ejaculation? a systematic review and meta-analysis. J Sex Med 2012;9:2404-16. [PubMed]
- Jannini EA, McMahon C, Chen J, et al. The controversial role of phosphodiesterase type 5 inhibitors in the treatment of premature ejaculation. J Sex Med 2011;8:2135-43. [PubMed]
- Başar MM, Yilmaz E, Ferhat M, et al. Terazosin in the treatment of premature ejaculation: a short-term follow-up. Int Urol Nephrol 2005;37:773-7. [PubMed]
- Cavallini G. Alpha-1 blockade pharmacotherapy in primitive psychogenic premature ejaculation resistant to psychotherapy. Eur Urol 1995;28:126-30. [PubMed]
- Sato Y, Tanda H, Nakajima H, et al. Silodosin and its potential for treating premature ejaculation: a preliminary report. Int J Urol 2012;19:268-72. [PubMed]
- Safarinejad MR, Hosseini SY. Safety and efficacy of tramadol in the treatment of premature ejaculation: a double-blind, placebo-controlled, fixed-dose, randomized study. J Clin Psychopharmacol 2006;26:27-31. [PubMed]
- Salem EA, Wilson SK, Bissada NK, et al. Tramadol HCL has promise in on-demand use to treat premature ejaculation. J Sex Med 2008;5:188-93. [PubMed]
- Kaynar M, Kilic O, Yurdakul T. On-demand tramadol hydrochloride use in premature ejaculation treatment. Urology 2012;79:145-9. [PubMed]
- Bar-Or D, Salottolo KM, Orlando A, et al. A randomized double-blind, placebo-controlled multicenter study to evaluate the efficacy and safety of two doses of the tramadol orally disintegrating tablet for the treatment of premature ejaculation within less than 2 minutes. Eur Urol 2012;61:736-43. [PubMed]
- Giuliano FA. Tramadol for the treatment of premature ejaculation. Eur Urol 2012;61:744-5. [PubMed]
- Ho CC. Re: David Bar-Or, Kristin M. Salottolo, Alessandro Orlando, James V. Winkler. A randomized double-blind, placebo-controlled multicenter study to evaluate the efficacy and safety of two doses of the tramadol orally disintegrating tablet for the treatment of premature ejaculation within less than 2 minutes. Eur Urol 2012;61:736-43. Eur Urol 2012;61:e23-4; author reply e25-6.
- Sunay D, Sunay M, Aydoğmuş Y, et al. Acupuncture versus paroxetine for the treatment of premature ejaculation: a randomized, placebo-controlled clinical trial. Eur Urol 2011;59:765-71. [PubMed]
- Wu X, Zhou Z. Re: Didem Sunay, Melih Sunay, Yasin Aydoğmuş, et al. Acupuncture versus paroxetine for the treatment of premature ejaculation: a randomized, placebo-controlled clinical trial. Eur Urol 2011;59:765-71. Eur Urol 2011;60:e27. [PubMed]
- Kwak TI, Jin MH, Kim JJ, et al. Long-term effects of glans penis augmentation using injectable hyaluronic acid gel for premature ejaculation. Int J Impot Res 2008;20:425-8. [PubMed]
- Abdallah H, Abdelnasser T, Hosny H, et al. Treatment of premature ejaculation by glans penis augmentation using hyaluronic acid gel: a pilot study. Andrologia 2012;44:650-3. [PubMed]
- Namavar MR, Robati B. Removal of foreskin remnants in circumcised adults for treatment of premature ejaculation. Urol Ann 2011;3:87-92. [PubMed]
- Buvat J. Pathophysiology of premature ejaculation. J Sex Med 2011;8:316-27. [PubMed]
- Graziottin A, Althof S. What does premature ejaculation mean to the man, the woman, and the couple? J Sex Med 2011;8:304-9. [PubMed]
- Moncada I. The importance of follow-up in patients with premature ejaculation. J Sex Med 2011;8:353-9. [PubMed]
- Jannini EA, Maggi M, Lenzi A. Evaluation of premature ejaculation. J Sex Med 2011;8:328-34. [PubMed]