Phalloplasty for the genetic male
Introduction
Indications for phalloplasty in the genetic male are bladder exstrophy, micropenis, aphallia, penectomy for carcinoma, traumatic amputation and severe corporeal contracture following explantation of infected penile prosthesis or secondary to refractory ischemic priapism.
Epispadias and bladder exstrophy can be defined as congenital malformations of the external genitalia and bladder in which there is failure or blockage of the normal development of the dorsal surface of the penis, abdomen and anterior bladder wall. The genital defect in male patients, also known as micropenis and epispadias, causes major functional and psychological problems (1).
Bladder exstrophy is a rare entity with an estimated incidence of 1/30,000 live births with a male to female ratio of 2/1 and represents a wide spectrum of malformations due to the abnormal development of the cloacal membrane, which causes a midline defect in the lower abdominal wall, a large defect in the anterior bladder wall and anomalies of the external genitalia that may vary significantly in severity among patients. In the most extreme cases the arrested development of the cloacal membrane leads urethral and rectal openings all sharing a common external orifice.
In the male, external genitalia abnormalities include short penis and epispadias. As the crura are inserted on the caudal aspect of the ischiopubic branches, which are laterally displaced, the corpora cavernosa only fuse at the distal portion of the shaft; the result is a wedge shaped short penis (1-3).
Surgical treatment in patients with bladder and cloacal exstrophy and micropenis-epispadias is a complex multi-stage procedure involving bladder closure with pelvic osteotomy in the first days of life, followed by penile reconstruction during the second year and a cervicoplasty at age 4-5 years to improve urinary continence.
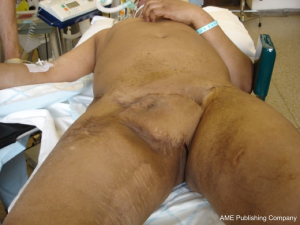
Genital reconstruction in patients with micropenis- epispadias and bladder exstrophy remains a challenge, as the goals of surgery are an acceptable cosmetic and functional result with the restoration of sufficient penile length for successful penetrative sexual intercourse (Figure 1).
The majority of techniques of penile lengthening involve mobilization of the corpora cavernosa and skin coverage with local flaps. Unfortunately these techniques are associated with a significant risk of neurovascular bundle damage with consequent loss of sensation and of blood supply and lead to the formation of short broad penises, inadequate for penetrative sexual intercourse in almost 50% of cases (1-8).
Micropenis, defined as a penis with as stretched length of less than 7 cm, can be idiopathic in nature or secondary to primary testicular failure, hypogonadothropic hypogonadism, defects in testosterone action or developmental anomalies (9).
Penile agenesis or aphallia is an even more rare malformation and is reported to occur in 1 in 30,000,000 births. Historically, gender reassignment was considered to be the most appropriate choice for these patients; however, although adequate cosmetic and functional outcomes have been reported, in a long term follow-up the majority of patients demonstrated a marked male psychological and psychosexual development. Therefore patients with aphallia should be raised as males and offered total phallic reconstruction, ideally during adolescence (10,11).
Squamous cell carcinoma (SCC) of the penis represents a rare malignancy in Europe and USA, with an incidence of less than 1 in 100,000. The treatment of SCC was historically based on partial or total penile amputation with formation of a perineal urethrostomy and closure of the penile stump with local skin flaps. These operations were based on the understanding that a 2 cm macroscopic margin is necessary for adequate oncological control (12-15) and resulted in a significant loss in sexual function. Patient satisfaction with their overall sexual life is less than 34% following penile amputation for carcinoma and therefore these patients represent the ideal candidates for total phallic reconstruction (16-18).
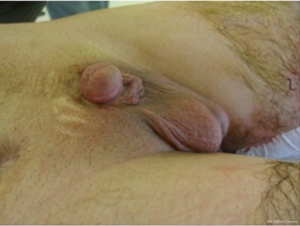
The real incidence of traumatic genital injuries has not been determined, however in civilian centres its expected to be low and that is the reason why most case series span many years and include relatively small numbers of patients. The scenario changes completely in the battlefield; this is consequence of the massive destruction caused by fragmentation devices combined with the use of protective torso armour, that has led to survival of soldiers with increasingly severe pelvic and genital organ injury. The surgical treatment of penile amputation involves microsurgical reimplantation of the penis only if the amputated part is adequately preserved. Otherwise the remaining stump is tailored and prepared for a delayed penile reconstruction (19,20) (Figure 2).
Also patients who have developed severe penile shortening and corporeal fibrosis following repeated explantation of infected penile prosthesis or due to refractory ischemic priapism may be candidates for total phallic reconstruction (21).
Phalloplasty techniques
Due to the unique anatomy of the penis, penile preservation should be always attempted leaving total phallic reconstruction as last resort. Therefore, patients who have an adequate penile length following partial amputation of the penis should initially be offered conservative management such as division of the suspensory ligament or excision of the suprapubic fat pad. Patients presenting with severely contracted corpora cavernosa following repeated explantation of infected penile prosthesis should instead be offered simultaneous total corporeal reconstruction with the use of acellular matrix grafts and penile prosthesis implantation as this technique yields good results in expert hands (21).
Total phallic reconstruction should be offered only if all conservative measures fail and the patient is not capable to resume penetrative sexual intercourse, to void while standing and to ejaculate inside the vagina, or in presence of severe psychological distress.
The complexity of the anatomy and physiology of the penis and the fact that there is no good substitute for the unique erectile tissue of the corpora represent the main obstacles for the reconstructive surgeon and despite a variety of surgical techniques have been described in the literature, none still fulfils all the ideal criteria and is currently universally accepted as ideal method (22-24).
The choice of the reconstructive technique should be tailored on patient’s expectations, body habitus and previous surgical procedures since thigh and forearm free flaps are associated with poor cosmetic result in obese patients due to the excessive thickness of the adipose layer and transverse lower abdominal scars may contraindicate the use of infraumbilical flaps. Also patients’ comorbidities must be taken into account since common cardiovascular risk factors such diabetes, hypertension, dyslipidaemia, obesity and cigarette smoke are associated with high risk of vascular complications and therefore represent relative contraindication to the use of free flaps.
Patients must be fully counselled about the pros and cons of each type of phalloplasty and must have reasonable expectations. Patients desired goals in terms of size, sensation, sexual and voiding function also play an important role in the selection of the type of flap as sensation and a patent neo-urethra can be achieved only with some techniques. Finally, donor site morbidity as well as the number of surgical stages necessary to complete the phalloplasty must be taken into consideration.
After many disappointing attempts with the use of infraumbilical flaps and musculocutaneous thigh flaps based on the gracilis muscle, the advent of microsurgical techniques has led to a new era for total phallic reconstruction (25). Although no controlled prospective randomized studies are available to confirm that the radial artery free flap (RAFF) phalloplasty is the best technique available, most Authors consider that it is extremely reliable and yields excellent cosmetic and functional results in very experienced hands (26-34). This multi stage procedure involves the creation of ‘a tube within a tube’ using forearm skin with the urethra fashioned from the non-hair bearing area and the whole flap based on the radial artery. Sensation is maintained due to the coaptation of the antebrachial nerves to the dorsal nerve of the penis and to the iliohypogastric and ilioinguinal nerves.
The most feared complication is acute thrombosis of the microsurgical anastomosis; this complication, if not identified and managed immediately leads invariably to the loss of the phallus. Although urethral complications such as strictures and fistulas can occur in around 30% of cases, correction is almost always possible and up to 99% of patients have been reported able to void standing from the tip of the phallus after revision surgery (30).
The RAFF has been widely used to create a phallus in female to male transsexuals. In these patients, as well as in patients with micropenis or aphallia the procedure is relatively easier as the abdomen and groins are usually relatively intact and therefore the radial artery can be anastomosed to the inferior epigastric, while the venous drainage from the flap veins is guaranteed by the anastomosis with the branches of the long saphenous vein.
The technique is slightly more complex in patients who have undergone previous amputation for carcinoma; although the proximal urethral stump is almost always readily available for primary anastomosis to the phallic urethra and the epigastric arteries are usually intact, the venous drainage may represent a challenge.
In particular, patients who have undergone bilateral radical lymph node dissection of the groin may have had the saphenous vein removed en block with the lymphnodes and therefore the flap veins are usually anastomosed with the dorsal vein of the penis, with the pampiniform plexus, or directly with the femoral vein (30).
The complexity of the reconstruction is highest in patients with bladder and cloacal exstrophy and micropenis- epispadias or who have experienced traumatic amputation. This because these patients have already undergone multiple previous reconstructive procedures and frequently present with severe scarred abdomen, groins and limbs.
In particular, patients with bladder and cloacal exstrophy and micropenis- epispadias have poor or absent epigastric arteries, either due to congenital defect or as a consequence of the previous multiple reconstructive procedures.
Furthermore, the urethra, which had been reconstructed with local flaps more than 10 years before and is not used for micturition, tends to be contracted and inadequate for primary anastomosis to the phallic neourethra. Although the majority of these patients voids through a Mitrofanoff or Montie type of continent urinary diversion and had had their bladder neck closed, anastomosis of the penile urethra with the phallic one is paramount to guarantee ejaculation from the tip of the phallus.
In patients with inadequate or absent epigastric artery, the radial artery is usually anastomosed to the superficial femoral artery with the interposition of a vein graft, which is usually harvested from the long saphenous vein. As this procedure requires an extra microsurgical anastomosis and therefore longer operating time, patients are at higher risk of postoperative complications such as thrombosis of the anastomosis.
In patients who have undergone total phallic reconstruction with the RAFF following amputation for carcinoma overall satisfaction can be as high as 97% with phallic sensation present in up to 86% of cases (30). Satisfaction rate is expected to be lower in patients with bladder and cloacal exstrophy and micropenis- epispadias or who have experienced traumatic amputation, as reconstruction is technically more challenging and therefore complications rate is higher (Figure 3). In particular, strictures and fistulas at the level of the join up between the penile and phallic urethra are more common in patients with bladder and cloacal exstrophy and micropenis- epispadias, as the previously reconstructed penile urethra tends to have a poor blood supply.
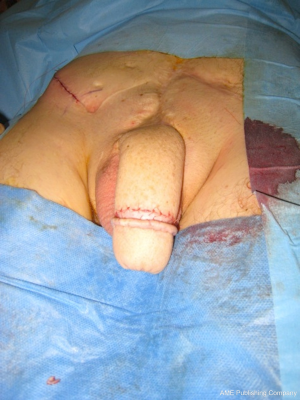
Implantation of an erectile device to guarantee the rigidity necessary for penetrative sexual intercourse is usually carried out at least one year after the creation of the phalloplasty when phallic sensation is likely to have developed.
As phalluses lack of tunica albuginea, penile prosthesis need to be housed in a synthetic sheath, usually Goretex or Dacron, in order to guarantee anchoring to the pubic bone and to prevent distal extrusion.
Frequently, patients who have undergone amputation for carcinoma or trauma present intact proximal corpora and therefore do not require a proximal synthetic sheath to be fitted on the rear aspect of the cylinders to guarantee their fixation to the pubic bone.
Due to the absence of the tunica albuginea and the necessity to use synthetic materials to house the cylinders, complication such as infection of the device, erosion and mechanical failure are common in patients with phalloplasty. In a recent series of 129 patients with phalloplasty who have undergone implantation of an erectile device, infection rate, erosion rate and mechanical failure of the device were respectively 11.9%, 8.1% and 22.2% and revision has been necessary in 41% of cases. Overall, after a median follow up of 30.3 months, up to 60% of patients had a normally functioning penile prosthesis and were able to cycle the device (35).
Various authors, in order to improve cosmesis and reduce the risk of urethral complications, have described modifications of the RAFF design.
In particular, the shape and dimensions of the flap should be tailored on the size of the arm and the length of the urethral and penile stump present.
If the original glans is present, it is usually left exposed at the base of the phallus, as the neurovascular bundle is not long enough to reach the tip of the phallus. Alternatively, the neurovascular bundle can be divided and the glans transferred with microsurgical technique to the distal aspect of the RAFF in order to guarantee superior cosmesis and sensation. In a series of 27 patients, after a median follow up of 10.3 years, Cheng et al. reported that all flaps had survived and that the sensation of the transposed glans was similar to the one assessed preoperatively (36).
The main drawback of RAFF is donor site morbidity; although this can be dramatically reduced by adequate preparation of the donor site for grafting and with the use of hair bearing FTG instead of their spit thickness counterpart, the resulting scar represents a stigma and can be poorly accepted by patients.
Despite free osteocutaneous fibular flaps (OFF), anterolateral thigh flaps (ALT), latissimus dorsi flap (LDF) and upper arm flaps have been introduced in order to minimize donor site morbidity, they are associated with poorer cosmetic results than the RAFF phalloplasty, and usually do not allow the creation of a neourethra with the tube within a tube technique (37-41).
Therefore, patients who wish to void from the tip of the phallus but do not accept a wide scar on the donor forearm can be offered the incorporation of a radial artery based free flap urethra (RAFFU) in a phallus previously fashioned with an infraumbilical flap. As previous abdominal scars are a contraindication to the use of infraumbilical flaps, this technique cannot be offered to patients with bladder and cloacal exstrophy and micropenis-epispadias or who have undergone extensive abdominal surgery.
This technique is easily reproducible in experienced hands and yields excellent cosmetic and functional results with all patients able to void standing from the tip of the phallus after revision surgery. Since the flap required is only a 4 cm wide, the resulting scar can be easily masked and therefore is more acceptable by the patients (42).
Conclusions
Total phallic reconstruction should be always offered to patients with penile inadequacy in order to allow them to void standing and engage in penetrative sexual intercourse; failure to do so will inevitably lead to severe psychological distress. Although no randomized controlled studies are available, various authors consider that the RAFF phalloplasty yields superior cosmetic and functional results. However, patients must be warned that multiple surgical stages are required and that revision rate can be high.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
References
- Woodhouse CR, Kellett MJ. Anatomy of the penis and its deformities in exstrophy and epispadias. J Urol 1984;132:1122-4. [PubMed]
- Vorstman B, Horton CE, Winslow BH. Repair of secondary genital deformities of epispadias/ exstrophy. Clin Plast Surg 1988;15:381-91. [PubMed]
- Varygin V, Bertonas S, Gurskas P, et al. Cloacal exstrophy: case report and literature review. Medicina (Kaunas) 2011;47:682-5. [PubMed]
- Mitchell ME, Bagli DJ. Complete penile disassembly for epispadias repair: the Mitchell technique. J Urol 1996;155:300-4. [PubMed]
- Hinman F Jr. A method of lengthening and repairing the penis in exstrophy of the bladder. J Urol 1958;79:237-241. [PubMed]
- Edgerton MT, Gillenwater JK. A new surgical technique for phalloplasty in patients with exstrophy of the bladder. Plast Reconstr Surg 1986;78:399-410. [PubMed]
- Gearhart JP, Leonard MP, Burgers JK, et al. The Cantwell- Ransley technique for repair of epispadias. J Urol 1992;148:851-4. [PubMed]
- Reiner WG, Gearhart JP, Jeffs R. Psychosexual dysfunction in males with genital anomalies: late adolescence, Tanner stages IV to VI. J Am Acad Child Adolesc Psychiatry 1999;38:865-72. [PubMed]
- Wood D, Woodhouse C. Penile anomalies in adolescence. ScientificWorldJournal 2011;11:614-23. [PubMed]
- De Castro R, Merlini E, Rigamonti W, et al. Phalloplasty and urethroplasty in children with penile agenesis; preliminary report. J Urol 2007;177:1112-6. [PubMed]
- Reiner WG, Kropp BP. A 7 years experience of genetic males with severe phallic inadequacy assigned female. J Urol 2004;172:2395-8. [PubMed]
- Smith Y, Hadway P, Biedrzycki O, et al. Reconstructive surgery for invasive squamous cell carcinoma of the glans penis. Eur Urol 2007;52:1179-85. [PubMed]
- Morelli G, Pagni R, Mariani C, et al. Glansectomy with split-thickness skin graft for the treatment of penile carcinoma. Int J Impot Res 2009;21:311-4. [PubMed]
- Pizzocaro G, Algaba F, Horenblas S, et al. EAU penile cancer guidelines. Eur Urol 2010;57:1002-12. [PubMed]
- Solsona E, Bahl A, Brandes SB, et al. New developments in the treatment of localized penile cancer. Urology 2010;76:S36-42. [PubMed]
- Garaffa G, Raheem AM, Christopher AN, et al. Total phallic reconstruction following amputation for carcinoma. BJU Int 2009;104:852-6. [PubMed]
- Romero FR, Romero KR, Mattos MA, et al. Quality of life after partial penectomy for penile cancer. Urology 2005;66:1292-5. [PubMed]
- D’Ancona CA, Botega BJ, De Moraes C, et al. Quality of life after partial penectomy for penile carcinoma. Urology 1997;50:593-6. [PubMed]
- Wessells H, Long L. Penile and genital injuries. Urol Clin North Am 2006;33:117-26. vii. [PubMed]
- Ralph D, Gonzalez-Cadavid N, Mirone V, et al. Trauma, gender reassignment and penile reconstruction. J Sex Med 2010;7:1657-67. [PubMed]
- Sansalone S, Garaffa G, Djinovic R, et al. Simultaneous total corporal reconstruction and penile prosthesis implantation in patients with erectile dysfunction and severe fibrosis of the corpora cavernosa. J Sex Med 2012;9:1937-44. [PubMed]
- Bogoras N. Uber die volle plastische wiederherstellung eines zum Koitus fahigen Penis (peniplastica totalis). Zentralbl Chir 1936;63:1271.
- Harrison RJ. Congenital absence of the penis with embryological consideration. Br J Plast Surg 1948;1:12-28. [PubMed]
- Bettocchi C, Ralph DJ, Pryor JP. Pedicled pubic phalloplasty in females with gender dysphoria. BJU Int 2005;95:120-4. [PubMed]
- Persky L, Resnick M, Desprez J. Penile reconstructionwith gracilis pedicled grafts. J Urol 1983;129:603-5. [PubMed]
- Chang TS, Hwang WY. Forearm flap in one-stage reconstruction of the penis. Plast Reconstr Surg 1984;74:251-8. [PubMed]
- Song R, Gao Y, Song Y, et al. The forearm flap. Clin Plast Surg 1982;9:21-6. [PubMed]
- Gilbert DA, Schlossberg SM, Jordan GH. Ulnar forearm phallic reconstruction and penile reconstruction. Microsurgery 1995;16:314-21. [PubMed]
- Garaffa G, Christopher AN, Ralph DJ. Total phallic reconstruction in female-to-male transsexuals. Eur Urol 2010;57:715-22. [PubMed]
- Garaffa G, Raheem AA, Christopher NA, et al. Total phallic reconstruction after penile amputation for carcinoma. BJU Int 2009;104:852-6. [PubMed]
- Selvaggi G, Monstrey S, Hoebeke P, et al. Donor-site morbidity of the radial forearm free flap after 125 phalloplasties in gender identity disorder. Plast Reconstr Surg 2006;118:1171-7. [PubMed]
- Lumen N, Monstrey S, Ceoulemans P, et al. Reconstructive surgery for severe penile inadequacy: phalloplasty with a free radial forearm flap or a pedicled anterolateral thigh flap. Adv Urol 2008.704343. [PubMed]
- Doornaert M, Hoebeke P, Ceulemans P, et al. Penile reconstruction with the radial forearm flap: an update. Handchir Mikrochir Plast Chir 2011;43:208-14. [PubMed]
- Ma S, Cheng K, Liu Y. Sensibility following innervated free radial forearm flap for penile reconstruction. Plast Reconstr Surg 2011;127:235-41. [PubMed]
- Hoebeke PB, Decaesteker K, Beysens M, et al. Erectile implants in female-to-male-transsexuals: our experience in 129 patients. Eur Urol 2010;57:334-40. [PubMed]
- Ma S, Liu Y, Chang T, et al. Long-term follow-up of sensation recovery of the penis reconstructed by Cheng’s method. Plast Reconstr Surg. 2011;127:1546-52. [PubMed]
- Rubino C, Figus A, Dessy LA, et al. Innervated island pedicled anterolateral thigh flap for neo-phallic reconstruction in female-to-male transsexuals. J Plast Reconstr Aesthet Surg 2009;62:e45-9. [PubMed]
- Papadopulos NA, Schaff J, Biemer E. The use of free prelaminated and sensate osteofasciocutaneous fibular flap in phalloplasty. Injury 2008;39:S62-7. [PubMed]
- Felici N, Felici A. A new phalloplasty technique: the free anterolateral thigh flap phalloplasty. J Plast Reconstr Aesthet Surg 2006;59:153-7. [PubMed]
- Garaffa G, Raheem AA, Ralph DJ. An update on penile reconstruction. Asian J Androl 2011;13:391-4. [PubMed]
- Garaffa G, Sansalone S, Ralph DJ. Penile reconstruction. Asian J Androl 2013;15:16-9. [PubMed]
- Garaffa G, Ralph DJ, Christopher N. Total urethral construction with the radial artery based forearm free flap in the transsexual. BJU Int 2010;106:1206-10. [PubMed]